The laboratory’s role in the transformation to patient-centered care
The “Patient.” The patient has finally re-emerged as the focal point in healthcare, after decades of being shunted aside by other major systemic concerns. It is a heartening development, and it is one in which the clinical laboratory is critical. Laboratories play a crucial role in caring for the patient; over 50 percent of electronic medical record (EMR) information is coming from lab data. In the context of the challenges of healthcare reform and payment changes which will reward value over volume, lab information is vital to providers in the management of their patients. Patient-centered care is the integration of all healthcare and clinical information for a patient, which is then portable to all providers of that patient’s care. The fundamental goal of patient-centered care is a higher quality of care that produces improved patient outcomes.
The challenge for laboratories, then, is how to adapt their business model to accommodate this new patient-centric model when all of their experiences have driven them to focus on volume/accessions. Accountable Care Organizations (ACOs) are structured to focus on the patient and all activities that involve cost management while adding value to patient care. Payment methodology impacts patient-centered care by paying for all services in the patient’s episode of care, which would include lab testing. In some risk-sharing or bundled payment models, this can be dangerous for labs if they do not demonstrate value beyond a reduced cost of the testing. Labs have an opportunity to contribute to improved value for the patient-centered care in many ways.
Patient-centered care: some relevant contexts
This begins with optimized workflow to collect correct patient demographics and insurance information, which is crucial to support health information exchange throughout the continuum of care. Laboratories have the opportunity to play a large role in data exchange with physician offices. The elimination of paper requisitions in favor of electronic connectivity helps in the containment of costs and error reduction. Errors can slow down processes and affect the entire patient encounter, not to mention negatively affect the filing of clean claims.
The communication of clinical information is less valuable if it doesn’t reflect accurate patient information. Errors create cost down the service line and can affect quality as well. For this reason the electronic health records’ (EHRs’) bi-directional connectivity to and from the lab/hospital system is vital to patient-centered care. The data repository of results helps to contribute to improved patient outcomes when this data is used as expanded clinical intelligence. Outreach programs help to drive the data exchange with physician offices while aligning physicians to the healthcare system. Without this connectivity, physicians will look elsewhere, to other labs that make ordering simpler and resulting into their EHRs a possibility.
The movement to adopt a unique master patient identifier that is utilized from any service source is another positive industry-wide consideration. Similar to a Social Security number, this patient identifier stays with the patient throughout his or her lifetime, regardless of where the service is performed or what IT system is being utilized. Without it, true data information exchange will not be complete.
However, there are numerous challenges attached to this solution. At the top of that list is assuring patient privacy. In addition, the adoption of the patient identifier must receive Congressional approval before it can be implemented. In the meantime many health systems have adopted an Enterprise Master Patient Index (EMPI), in which the patient has the same identifier regardless of which hospital or service within the health system the patient originates.
The central data repository must be inclusive of clinical information. A longitudinal record for the patient would represent a complete medical history and all clinical data for the patient regardless of place of service. The comprehensive record is achieved via Health Information Exchange (HIE) connectivity which brings together multiple disparate systems. As an example, if a patient has testing as an outpatient, or in an emergency department, has an ambulatory surgery procedure, or was recently hospitalized in another hospital within the system, all of the results associated with those encounters must be available to the practitioner in one longitudinal record. This is value-add in patient-centered care, and the lab plays a role in its contribution. The EMPI is essential to overcome the patient type challenge. With the EMPI, it will be easier to manage and optimize care by tracking all tests in the data repository. The integration of the data from various disparate systems requires connectivity solutions that cross these boundaries. There are challenges with varied terminologies within each system, but solutions to cross-map the translations are possible.
Patient-centered care: the lab’s contribution
Knowing this, what can the laboratory do to contribute to patient-centered care?
- Start by eliminating or significantly reducing paper test ordering requisitions and replacing them with electronic order entry to significantly reduce errors and streamline efficiencies to add value. Evaluate the connectivity that currently exists with ordering provider systems and work to extend connectivity to other providers that currently are still on paper. Consider a middleware provider to connect EHRs to your LIS instead of individual proprietary interfacing. It is faster to deploy and should be a less expensive route.
- Be involved with clinical decision support committees to help further develop the Computerized Physician Order Entry (CPOE) capabilities and maximize right test, right time automated ordering aids. Often the lab and pathologist are not a part of order set formulation. Explore what committees exist and insert a lab representative where applicable.
- Know that test utilization management is a key component of patient-centered care, and have a formal program in place to aid providers. Improve the testing performed for the patient while reducing costs by utilizing algorithms: clinical pathways based on data. Again, pathologists need to be involved with variation of care solutions.
- Review front-end error processing reports to better understand the type and source of ordering errors. Work with your Information Technology (IT) team to build rules that minimize errors such as duplicate test orders, date-of-birth issues, and demographic issues, or purchase third-party connectivity solutions that have robust rules already built into their software. Additionally, work with your staffed Patient Service Centers (PSCs) to hold them accountable for getting accurate and complete information upfront. Take every advantage of having the patient available, and get the data correct. Tie in an eligibility check to this process as well.
- Be aware of having duplicate patient records and work to minimize and eliminate this. Utilize multiple identifiers that match to confirm a particular patient record to include components other than just name and date of birth.
- Have a mechanism for the PSC staff to view patient balances within the health system, and develop stringent co-pay collection policies, which further extends to patient-centered care to pull in billing capabilities.
- With regard to the actual Lab report, be sure to include all recent encounters regardless of patient type for a longitudinal view of the record. Have this data contribute to the central repository of the patient record, which is visible from all operational workflows.
- Utilize the test results in advanced strategies to add value to providers. Focus on alerts to help better predict the potential for readmission. Help providers and case managers determine if any additional testing or abnormal results have occurred post discharge.
- Use technology and data to deliver value:
- Help your providers by flagging patients at risk.
- Offer special questionnaires around disease states within your ordering template.
- Support clinical intelligence dashboards that go beyond the test result itself, which will help to reduce costs and translate into better care.
- Use your test report formats to educate for appropriate test utilization and new
testing. - Develop actionable insight data sets to improve quality of care at the patient level.
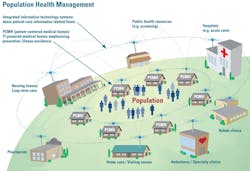
- From a global perspective, utilize data to contribute to proactive population health considerations. Key to data sharing for population health is “big data” management; the Lab contributes significantly to that volume of data (Figure 1). Know that a patient portal is an excellent resource for patient-centered care that allows patients to access to their results, review and correct their information, and even pay their bills.
- “Lean” processes to eliminate waste and reduce costs by minimizing variation to be better positioned within the ACO environment.
- Have a seat at the table with ACO formation to demonstrate the value of the Lab in the patient-centered care focus.
Patient satisfaction is also an important component of patient-centered care. Patients have more tools today to stay informed and contribute to their care. Labs should look for ways to enhance the patient experience, either online or in person, by providing more information and streamlining processes. Consider…how can the registration process be improved? How does the patient bill look? Is it understandable, accurate, and consolidated? Multiple bills can be confusing to patients and decrease their satisfaction, although the practice today is very prevalent. Patients themselves, and their contribution to their own care, cannot be an overlooked component of patient-centered care.
All of these building blocks will contribute to a developed patient-centered care focus and help any laboratory move in the right direction for the future while ultimately impacting the quality of patient care. The laboratory plays a pivotal role in the creation of meaningful clinical information, impacting the diagnosis and treatment of patients. Labs should help to build upon a solid patient-centered care foundation by decreasing errors, contributing to improving quality outcomes, and operationally modifying workflow processes to reduce costs and improve patient and provider satisfaction. Successful labs will plan and position for the future reimbursement changes, leveraging provider relations and current connectivity to define their value in the shift to patient-centered care model.