In an effort to educate MLO readers about the “start-to-finish” activities of an organization engaged in the “flu business,” we asked
Gregory R. Chiklis, PhD, vice president, Research and Development,
ZeptoMetrix Corp. (ZMC) to address the biosafety laboratory and
seroconversion panels, as well as the exact nature of the work of a
company like ZeptoMetrix and how that work plays a role in finding
solutions to influenza threats. Here are his responses:
Q In one of your company newsletters, a
section features ZMC’s Biosafety Level 3-plus (BSL3+) laboratories. Can
you reveal more of what it would take for a laboratorian wanting to move
into your segment of the marketplace to qualify to be one of the people
who could actually work in the BSL3+ lab? When this material was
published two years ago, the article mentioned changes in this BSL-3+
lab. Have those changes been achieved, and is the lab now handling the
viruses and bacteria mentioned in the article (e.g., lethal primate
viruses, avian flu, and mumps/measles, and anthrax and pertussis)?
A Our biological containment laboratories were
upgraded last year to BSL3+ enhanced status to support both our work
with highly pathogenic organisms, including avian flu, and a contract
awarded to the company to develop several testing panels of flu and
related organisms for the Centers for Disease Control and Prevention
(CDC). This upgrade included the addition of shower-in/shower-out
stations and incubators for propagating flu viruses in eggs, as well as
real-time polymerase chain reaction (PCR) equipment used to follow the
growth of the viruses in culture.
To support these upgrades, we also required
additional training for our staff; a new set of emergency-response
plans; employee security screening; an upgrade to our select-agent
license; and the development of a disaster-recovery plan. This was no
small task and took about six months to get in place.
The time between exposure to SARS-CoV and the onset of
symptoms is called the “incubation period.” The incubation period
for SARS is typically two to seven days, although in some cases, it
may be as long as 10 days. In a very small proportion of cases,
incubation periods of up to 14 days have been reported. —www.cdc.gov/ncidod/sars/faq.htm.
In order to work in our BSL3+ laboratories, an
employee must be at least 18 years old, have earned a bachelor’s degree
in a science-related field, and have no criminal record. All laboratory
personnel also go through a Security Risk Assessment conducted by the
FBI, which includes fingerprinting and a complete background check.
Additional experience in the areas of cell culture, molecular biology,
and Good Manufacturing Practices, or GMP, are also a plus. Regardless of
our scientific backgrounds, we enter all new employees into a six-month
training program to work in this laboratory. Once this training is
complete, there are monthly training and drills that must also be
accomplished to maintain the employee status for working in the
laboratory.
CONTINUING EDUCATION
To earn CEUs, see current test at
www.mlo-online.comunder the CE Tests tab.
LEARNING OBJECTIVES
Upon completion of this article, the
reader will be able to:
- recognize personnel requirements for ZMC’s Biosafety Level 3+ lab;
- recognize the biological agents that ZMC handles, and the tests and
processes performed on these agents to make them available for outside
use; - discuss the next probable pandemic predicted by ZMC and the
rationale for the choice; and - recognize structures and genetics of influenza viruses,
incubation period for SARS, and disease and death rates for
influenza and HIV.
With our CDC work in this area concluded, we are
now using these upgraded facilities to support influenza and
respiratory-virus vaccine and diagnostic-test development through the
supply of various organisms, testing services, and finished products.
Our main work involves the manufacture of multiple strains of flu virus
and related respiratory organisms. These are used to check the
sensitivity and specificity of tests being developed to detect these
pathogens. In addition to this work, we are also providing kit
manufacturers with calibrators and controls for both their antigen- and
molecular-based diagnostic tests. These controls are formulated into
refrigerator-stable non-infectious materials that allow the technician
to validate testing while remaining safe when working with these highly
pathogenic organisms.
Another area supported by this laboratory is the
proficiency-testing industry through its bulk manufacturing of these flu
strains into testing panels. Using the same inactivation technologies
described above, we have manufactured and direct shipped more then 4,000
non-infectious influenza-based panels worldwide to monitor the
performance of clinical-testing laboratories.
Q In Spring 2006, the company was
collaborating with the CDC regarding HIV seroconversion panels. The
explanation of this process is relatively simple; however, 1) is ZMC
still involved in this collaboration; 2) has ZMC launched the hepatitis
B and C virus panels mentioned in this article; and 3) has there been a
change in the process by which donors are eliminated, thus making
seroconversion panels difficult to construct?
A Diagnostic-test developers are always trying
to reduce the time between infection and detection, and seroconversion
panels are the perfect tool to accomplish this. A seroconversion panel
is a longitudinal series of donor-plasma samples that spans the
infection process. In the early samples, the donor’s blood tests remain
normal. Then, as the infection progresses, samples begin to exhibit the
various diagnostic markers related to that particular pathogen, and the
immune system’s response against it. Final sample bleeds will contain
disease-specific antibodies, completing the seroconversion process.
These longitudinally collected samples represent one of the last ways to
examine discreet snapshots in time of the immune system’s response to
infection. Our company and our reference-laboratory partners run these
panels on every available test kit on the market to compare their
detection of the various molecular-, antigen-, and antibody-based tests
in these early-stage infections. These panels are sold to the
diagnostic-testing industry, vaccine manufacturers, and regulatory
authorities worldwide.
A year ago in the fall, the CDC sponsored a
workshop to establish new testing guidelines to confirm if a person is
infected with HIV-1. While this was first established 20 years ago,
there are now many new technologies on the market that are more
sensitive then the older first-generation assays. The only way to get an
accurate assessment of the capabilities of current tests was to run and
compare them using seroconversion panels. For this program, we donated
about 60 of our HIV panels to the CDC for evaluation of all the new
HIV-testing formats. The data analysis is still in process for this
project, and we hope to see some new guidelines for qualifying a donor’s
HIV status by the end of 2009.
Since blood donations are now screened by
molecular-testing technologies that can measure the RNA or DNA of the
infecting virus, blood samples that seroconvert completely to Ab
positive are no longer found in the plasma-collection centers. This is
because they are deferred from the collection centers before they
complete the seroconversion process. Using these new molecular-testing
techniques, not only can we now detect copies of virus in people well
before their own immune system recognizes the infection but also remove
those virus copies earlier from the blood supply, making the blood safer
than it has ever been.
Q In Spring 2007, ZMC was engaged in
another contract with CDC to help combat H5N1 avian influenza. While you
have said this contract is no longer in force, can you tell us whether
or not you are still growing the 151 different viruses including 36
different strains of H5N1? Can you give us a list of all of the viruses
that your company currently handles in one way or another?
A You are correct in that the CDC cancelled our
contract before we reached the point of growing avian flu. They are now
releasing a new contract that is much more encompassing and that will
cover all aspects of flu diagnostics including virus growth, diagnostic
development, and a “storefront” for researchers to purchase these
reagents for their work.
Currently, there are more then 20 companies
collaborating with ZMC towards the development of flu and respiratory
diagnostic tests. For these projects, we are growing hundreds of strains
to support their test development and formulating various controls,
calibrators, and validation panels to be used with their test kits. The
Food and Drug Administration (FDA) also released a guidance document on
how to validate respiratory-based molecular tests, and we are working to
have all of the strains the FDA currently requires available for
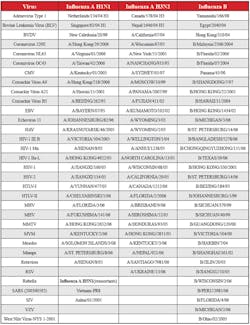
researchers. [See a list of some strains on page 28 that ZMC currently
supplies these developers.]
As of January 2006, the Joint United Nations Programme on
HIV/AIDS (UNAIDS) and the World Health Organization (WHO) estimated
that AIDS has killed more than 25 million people since it was first
recognized on Dec. 1, 1981, making it one of the most destructive
pandemics in recorded history. —
www.cdc.gov/ncidod/sars/faq.htm.
Q In one of your newsletters, bubonic
plague is mentioned; could it or other ancient/obscure viruses or
bacteria cause a threat somewhere in the world? What do you perceive as
the major pandemic threat today and why? Are you able to tell us what
bioterrorism agents ZMC handles? In terms of your biodefense activities,
is that a larger portion of your business than working with
public-health issues?
A I still think the major pandemic we could see
in the coming years will come from avian influenza. Unlike past
pandemics, however, we are able to track outbreaks globally, which gives
us the time to quickly develop diagnostic tests specific for the strain
— hopefully, before it spreads too far. By identifying these pandemic
strains early, we can intervene and reduce the damage they cause. This
is a similar concept to that of the SARS outbreak several years ago. As
soon as the virus was identified, researchers at the CDC developed a
test while we at ZMC developed safe, inactivated molecular and serology
(antibody-based) controls from virus provided to us from the CDC. These
controls and proficiency materials were quickly distributed to prepare
the labs for testing for this virus. These tests were then run at
various locations across the globe, allowing the infected donors to be
identified and isolated from the general population until they could be
treated and released. While a pandemic-flu virus will be harder to
isolate because it is airborne, we could follow this same scheme for
getting the tests prepared and validated, should this ever occur. As for
our biodefense work, we are not at liberty to identify any of the
organisms or how they are being used except to say that they are
proficiency-testing materials that a biodefense laboratory would run to
make sure they can accurately test and identify a biowarfare agents.
Are we due for another pandemic?
A flu pandemic occurs when a novel but normal
genetic mutation exists in a strain of circulating influenza. With the
age of rapid international air travel, a pandemic is more of a threat
today than it ever was. Three major influenza pandemics occurred during
the 20th century: the “Spanish” flu in 1918-1919; the “Asian” flu in
1957-58; and the “Hong Kong” flu in 1968-69.
Spanish flu, the most deadly of the three major
pandemics, caused approximately 500,000 deaths in the United States
alone, and 40 to 50 million deaths across the globe. This highest
mortality was among persons from 25 to 30 years of age. Deaths may have
been higher but may not have been documented due to restrictions during
World War I. First discovered in the Far East, the Asian flu caused
about 70,000 deaths in the United States and 2 million deaths worldwide.
With better diagnostics, the Asian flu was identified earlier on and was
contained better than the Spanish flu.
The Hong Kong flu resulted in 34,000 deaths in
the United States and about 1 million deaths in total. As a result of
its similarity to the Asian strain, many people may have developed an
immunity. This flu abated when schools were closed, so it did not spread
easily, proving the value of containment. By this time, other medical
advances also enabled the outbreak to be handled and treated more
effectively.
In 1997 and 1999, influenza pandemic “scares”
occurred due to novel strains of avian influenza, a virus that moved
directly from chickens to people, bypassing an intermediary host, such
as a pig. Slaughtering potentially infected fowl resulted in quick
containment of any outbreak.
While the CDC report that the spread of avian
influenza (H5N1) from person to person has been rare, this epizootic
continues to pose an important public-health threat. If the virus
eventually is transmitted from person to person, a potential pandemic
could develop.
The threat of the first pandemic in the 21st
century means that continual progress in research and development is
essential. Today, patented technologies can inactivate viruses so they
are safe to handle in a normal laboratory environment. The viral genome
remains unmodified and intact, better reflecting the normal state of the
viral agent.
This is an important aspect for rapid development
of new diagnostic tests and therapeutics for pathogenic organisms, as it
gives researchers unparalleled access to viral pathogens without the
need for specialized high-level containment laboratories. This
technology enables the shipment of inactivated influenza proficiency
samples to more than 4,000 diagnostic testing facilities to assess their
ability to accurately screen and report influenza infections. —ZeptoMetrix’ZeptoGram
Spring 2007
Faster, more sensitive flu tests to combat flu pandemic
By Graham Lidgard, PhD
Faster and more sensitive tests for influenza —
particularly the avian-flu subtypes H5N1, H7N1, and H9N1 — are being
developed for the CDC. These tests (being developed under contract by
private industry) are expected to be commercially available in the next one
to two years. The CDC, working with health agencies in the United States and
other countries, has adopted a three-pronged Advanced Development Program
for combating influenza outbreaks — early detection and containment,
combined with ongoing vaccination programs and antiviral treatments —
explains Daniel B. Jernigan, MD, MPH, deputy director of the CDC Influenza
Division. The new diagnostic tests, both point of care (POC) and molecular,
will be integral components of this global effort to forestall or
significantly reduce the severity of a flu pandemic. The molecular tests
could be performed in a hospital or a commercial laboratory, and would
expedite the diagnosis of large numbers of patients. The expanded testing
capability enhances the hospital laboratory-based pandemic and seasonal-flu
diagnostic capacity in the United States.1
HIV is a retrovirus that can lead to AIDS. Currently, there are
an estimated 1,039,000 to 1, 185,000 people in the United States living
with HIV/AIDS, with 24% to 27% undiagnosed and unaware of their HIV
infection.—http://en.wikipedia.org/wiki/HIV,
and
www.cdc.gov/hiv
Early detection and intervention is critical because
vaccinations usually are not effective when new strains suddenly arise and
begin spreading within the population and, so, are not as effective as
health officials would like. The efficacy of a flu vaccine depends on how
well it is matched to the types of flu viruses circulating that year.
Scientists try to predict which strains of flu viruses are most likely to
spread and cause illness each year, and put these new strains into the
vaccine. The 2008-2009 influenza vaccine, for example, contains three new
influenza virus strains: A/Brisbane/59/2007 (H1N1)-like virus;
A/Brisbane/10/2007 (H3N2)-like virus; B/Florida/4/2006-like virus.2
But those who contract the disease from a different strain are not protected
— although the vaccine may make the illness milder. Moreover, it takes
months to develop a new vaccine to combat mutated virus strains. By the time
a novel virus is identified, a flu pandemic could be unleashed before a
targeted vaccine is available.
While rapid diagnostic tests are available to detect
influenza viruses, none of the tests provide any information about influenza
A subtypes. Additionally, these rapid tests differ in the types of influenza
viruses they can detect and whether they can distinguish between influenza
types. Some tests can detect only influenza A viruses; or they detect both
influenza A and B viruses but do not distinguish between the two types.3
In addition, current molecular flu tests take hours and, in some instances,
days to obtain results, depending on the type of test and medical-laboratory
facilities available, particularly in remote regions of the world. The time
lost can make the difference between quickly stamping out an exposure and
seeing its uncontrolled spread.
New subtypes are responsible for pandemics and can
result from the mutation of human- and avian-influenza viruses. Antigenic
changes within a type or subtype of A and B viruses, known as antigenic
drift, are ongoing processes responsible for frequent epidemics and regional
outbreaks, and these changes make the annual reformulation of influenza
vaccine necessary.4 To date, these formulations do not include
the avian-flu subtype.
Avian H5N1-virus infections of humans are rare, and
most cases have been associated with direct poultry contact during poultry
outbreaks. While the H5N1 virus does not now infect people easily, infection
in humans is serious when it occurs — more than half of people reported to
be infected have died.5
A major concern, however, is that the deadly H5N1-flu
strain will mutate into a virus capable of human-to-human transmission and
lead to an influenza pandemic. There is little pre-existing natural immunity
to H5N1-virus infection in the human population. If the H5N1 virus gains the
ability for efficient and sustained transmission among humans, an influenza
pandemic could result, with potentially high rates of illness and death
worldwide.6 Without intervention, health officials expect a
mutated flu virus to spread internationally within one month and U.S. cases
in one to two months, according to Martin Cetron, MD, director of the CDC’s
Division of Global Migration and Quarantine.6
To improve the odds on early detection and
containment, the CDC has funded the development of more sensitive and faster
tests that can be used in the field or small labs to speed up the detection
process and begin immediate intervention. In late 2006, the CDC awarded
$11.4 million to four companies to develop new rapid diagnostic tests that
will detect seasonal human-influenza viruses and differentiate influenza A
H5N1 from those within 30 minutes.7 These tests should begin
coming to market next year. Two of the firms terminated their contracts with
the CDC; the two remaining companies include Meso Scale Diagnostics LLC, of
Gaithersburg, MD, using multi-array biomarker detection, and Nanogen Inc.,
of San Diego, CA, using a novel POC immunoassay system developed in
collaboration with HX Diagnostics.
Existing POC tests can only determine if the patient
is infected with influenza viruses A or B but cannot differentiate seasonal
subtypes from avian influenza H5N1. To test for H5N1, patient samples must
be sent to one of about 100 designated labs nationwide. The process can take
four to 24 hours to complete, depending on the shipping of samples.8
New POC assays, such as those developed through the
CDC grants, will be designed to show good reactivity across seasonal changes
in current subtypes. If a loss of detection for a seasonal subtype is seen,
it will serve as an indication that a new subtype has entered the human
population, which often brings significant human disease with it. This
sentinel approach is intended to provide an additional tool to identify
significant changes in viral subtypes soon after they emerge. In addition to
these contracts, CDC is providing funding for a repository of influenza
reagents and other materials to aid with the advanced development of these
POC diagnostics. Buffalo, NY-based ZeptoMetrix received a contract from the
CDC to create a secure collection of influenza viruses, including the
avian-flu virus.
H5N1 is a subtype of Influenza A virus. It refers to the
subtypes of surface antigens present on the virus: hemagglutinin type 5
and neuraminidasetype 1. —www.wikipedia.com.
While POC tests are valuable, sensitivity is limited
to about 75%. A more sensitive test requires molecular diagnostics. Earlier
this year, the CDC awarded Meso Scale Diagnostics and Nanogen second
contracts for the development of low-cost influenza tests that can detect
and differentiate seasonal human-influenza viruses from avian influenza
within three hours. Currently, the process for testing for avian influenza A
(H5N1) can take up to 24 hours.8 Meso Scale develops and markets
high-throughput diagnostic tests that allow large numbers of tests to be
conducted at once. The company bases its products on a proprietary
combination of electrochemiluminescence detection and patterned arrays.
Nanogen, using proprietary minor groove binder (MGB)
probe technology for real-time PCR, will develop a fast molecular test that
simultaneously detects and differentiates Type A, Type B, seasonal flu (H1N1
and H3N2) strains, and respiratory syncytial virus, or RSV. The target is to
achieve 90% to 95% sensitivity. The contract also provides for a secondary
“reflex” test for three avian-flu strains (H5N1, H7N3, and H9N2) to be
available for samples that are determined to be positive for flu A but
negative for seasonal flu.
The test is being developed in partnership with the
Medical College of Wisconsin and HandyLab Inc. It will be significantly more
sensitive than current rapid flu tests and is expected to be conducted in
less than half the time it takes to run current molecular tests. The company
anticipates the use of off-the-shelf instrumentation for sample handling and
detection. When these new tests emerge from the pipeline, the medical labs
on the frontline of early detection will have more powerful tools than ever
to battle a flu pandemic.
Graham Lidgard, PhD, is the senior vice president,
Research and Development for Nanogen Inc., in San Diego, CA.
References
1. US Department of Health and Human Services. HHS
Awards Contracts for the Development of Faster Influenza Diagnostic Tests.
12 June 2008.
http://www.hhs.gov/news/press/2008pres/06/20080612a.html. Accessed
September 15, 2008.
2. Centers for Disease Control and Prevention. CDC
Media Briefing: Influenza Vaccine Effectiveness. Published April 17, 2008.
http://www.cdc.gov/media/transcripts/2008/t080417.htm. Accessed
September 15, 2008.
3. Centers for Disease Control and Prevention. Role
of Laboratory Diagnosis of Influenza. Published September 26, 2006.
http://www.cdc.gov/flu/professionals/diagnosis/labrole.htm. Accessed
September 15, 2008.
4. Centers for Disease Control and Prevention.
Interim CDC-NIH Recommendation for Raising the Biosafety Level for
Laboratory Work Involving Noncontemporary Human Influenza Viruses. Published
October 6, 2005.
http://www.cdc.gov/flu/pdf/h2n2bsl3.pdf. Accessed September 15, 2008.
5. Centers for Disease Control and Prevention. Avian
Influenza: Current H5N1 Situation. Published June 15, 2007.
http://www.cdc.gov/flu/avian/outbreaks/current.htm. Accessed September
15, 2008.
6. Cetron M, MD. Non-pharmaceutical Strategies to
Limit Spread of Pandemic Influenza.
http://www.cdc.gov/flu/avian/pdf/non-pharmaceutical_intervention.pdf.
Accessed September 15, 2008.
7. Centers for Disease Control and Prevention. CDC
Awards $11.4 Million to Develop New Rapid Diagnostic Tests for Avian
Influenza. 4 December 2006.
http://www.cdc.gov/media/pressrel/r061204.htm?s_cid=mediarel_r061204_x.
Accessed September 15, 2008.
8. Centers for Disease Control and Prevention.
HHS Awards Contracts for the Development of Faster Influenza Diagnostic
Tests. Published June 12, 2008.
http://www.hhs.gov/news/press/2008pres/06/20080612a.html. Accessed
September 15, 2008.
“As the market demands faster turnaround times with higher sensitivity
and specificity, we see the market evolving over time to molecular
product platforms. This will be particularly evident in infectious
diseases in general and critically important with influenza where
diagnosing early and accurately can lead to better patient management.”
— Caren L. Mason
President and CEO
Quidel Corp.
Maker of QuickVue Influenza A+B
“Bringing automation to the reading of influenza tests is a key factor
for the next generation of rapid flu tests. Automating and storing the
objective result of a flu test will help increase laboratory
productivity and minimize the potential for human error, which can
contribute to improving patient outcomes.”
— Patrick Parks,
MD, PhD
Advanced Division Scientist
3M Health Care
Saint Paul, MN
Maker of 3M Rapid Detection Flu A+B Test
“As we head into the 2008-2009 respiratory season, both flu and
pneumonia will be present. Streptococcus pneumoniae is
the most common cause of bacterial pneumonia and is most often a serious
complication of the flu. So, when patients present with respiratory
issues, it is prudent to test for both flu and pneumonia to improve
patient outcomes in many cases.”
— Dotty
Peterson, Director of Marketing
Rapid Diagnostics, Inverness Medical
Maker of BinaxNOW Influenza and
BinaxNOW Streptococcus
pnuemoniae
“Molecular tests for respiratory viruses are an
exciting development in laboratory medicine. We know that viruses cause
about 80% of respiratory infections, yet these viruses are rarely tested
for or diagnosed. With new molecular tests, we can identify the cause of
an infection efficiently and effectively so doctors can prescribe the
right treatment quickly. Moreover, these tests allow us to detect virus
outbreaks early and better understand what pathogens are circulating in
our communities.”
— Jeremy
Bridge-Cook, PhD
Vice President
Luminex Molecular Diagnostics
Maker of the xTAG Respiratory ViralPanel
“Molecular methods are rapidly displacing viral
culture as the ‘gold standard’ for respiratory viruses due to the speed
and accuracy of molecular methods. Within the next three to five years,
molecular testing for respiratory viruses will be considered standard of
care. Most of this testing will be based on the real-time PCR platform
which offers the advantages of ease-of-use, high sensitivity, and
minimal risk of contamination. This platform will become even more
automated as fully-integrated systems move into the marketplace.”
— Steve Visuri,
PhD, Chief Science Officer
Prodesse Inc.
Maker of ProFlu+, Pro hMPV+, and ProParaflu+
Observations on viruses
ViraCor Laboratories was the first national
clinical laboratory in the United States to offer the xTAG Respiratory
Viral Panel (RVP), a unique test that, from one patient sample, can
simultaneously detect the 12 viruses and subtypes that are responsible
for more than 85% of respiratory viral infections.
ViraCor immediately began running the test
following the FDA 510K clearance in January of 2008. Analyzing the first
six months of data from the xTAG RVP test has yielded interesting
observations, since the test provides a much larger clinical picture
than previously available. While the company’s observations are
anecdotal and, therefore, cannot provide true incidence rates, the
findings provide a unique perspective on pathogens circulating
nationwide. Some observations include:
- ViraCor observed the presence of all 12 viruses and subtypes.
- Rhinovirus was the most prevalent pathogen detected in patients,
followed by Human Metapneumovirus. - The pathogens were not commonly tested for before the launch of
xTAG RVP. - A larger than anticipated number of dual and triple infections
was observed, with 75% of dual infection combinations containing
rhinovirus. Studies have shown rhinovirus can cause severe and fatal
lower respiratory-tract infections, especially in elderly and
immunocompromised patients; it also has been associated with graft
dysfunction in lung-transplant recipients.
Human Metapneumovirus prevalence was much higher
than expected, and the virus was distributed throughout all age ranges.
The newly discovered virus is similar to RSV in clinical presentation,
with serious ramifications in the pediatric and immunocompromised-patient
population, as it has been associated with allograft rejection in
transplant patients.
MLO’s
Continuing Education Test is available online only.
Print out and mail a copy with your check, or use the new online CE test
and convenient online payment feature available through the auspices of
Northern Illinois University.
Go to www.mlo-online.com and
look under CE Tests.