The silent pandemic is no longer silent
Since the introduction of penicillin in 1942, antimicrobials have transformed the treatment of infections and have saved millions of lives. But decades of misuse and outdated guidelines have driven a rise in the organisms that are resistant to these lifesaving drugs.
Antimicrobial resistance (AMR)—bacteria’s ability to overcome the effects of the drugs designed to kill or disarm them—is one of the world’s greatest public health threats. Today, at least 1.27 million deaths worldwide are attributed to resistant bacterial infections per year, and this number is growing.1
According to the Centers for Disease Control and Prevention (CDC), in the United States alone, more than 2.8 million antibiotic-resistant infections occur each year; in fact, someone dies every 15 minutes from a drug-resistant infection.2
As it continues to increase rapidly across the world, AMR is considered a “silent pandemic,” which actually threatens modern medicine. As the pathogens that cause infections become increasingly drug-resistant, common medical procedures—including surgery, childbirth, and chemotherapy—will become increasingly life-threatening. Put into perspective, if left unabated, the effects of AMR could be worse than COVID-19.3
Future projections suggest AMR could result in millions of deaths and trillions of dollars in lost global production.4
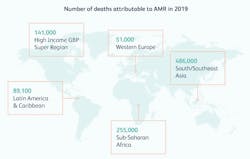
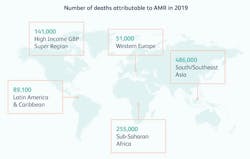
A recent publication, Global burden of bacterial antimicrobial resistance in 2019: a systematic analysis, provided in-depth insights into the global burden of drug resistant infections. It is a comprehensive assessment of the global burden of AMR, as well as an evaluation of the availability of data. The paper uses several sources for the data and an estimation model to determine rates for regions that did not have complete data resources. In total, 471 million individual records or isolates covering 7585 study-location-years were used as input data to the estimation process.There were an estimated 4.95 million (3.62–6.57) deaths associated with bacterial AMR in 2019, including 1.27 million (95% UI 0.911–1.71) deaths attributable to bacterial AMR. This data clearly demonstrates that bacterial AMR is a leading global health issue. These numbers also make AMR more deadly than such leading infectious disease threats as malaria and HIV/AIDS.The analysis showed that AMR all-age death rates were highest in some low and low middle income countries (LMICs), making AMR not only a major health problem globally but a particularly serious problem for some of the poorest countries in the world.
A broad analysis of pathogens causing disease was completed. There were six AMR pathogens that caused 929,000 of the 1.27 deaths attributable to AMR. The six pathogens responsible for more than 250,000 deaths associated with AMR were E coli, Staphylococcus aureus, K pneumoniae, S pneumoniae, Acinetobacter baumannii, and Pseudomonas aeruginosa, by order of the number of deaths. The prevalance of these pathogens, however, varied by region. In the high-income super-region, approximately half of the fatal AMR burden was linked to two pathogens: S aureus and E coli. By contrast, in sub-Saharan Africa, the leading pathogens were distinct from those of the high-income super-region, and each represented a smaller share of the AMR burden; S pneumoniae contributed to 15.9% of the deaths attributable to AMR and K pneumoniae contributed to 19.9% of the deaths attributable to AMR.
Three infectious syndromes dominated the global burdens attributable to and associated with AMR in 2019. The syndromes were lower respiratory and thorax infections, bloodstream infections, and intra-abdominal infections. Combined, these three syndromes accounted for 78% of deaths attributable to AMR in 2019; lower respiratory infections alone accounted for more than 400,000 attributable deaths and 1.5 million associated deaths.Now we have the data, what are the actions we need to take
In conclusion, the authors of the paper noted, understanding the burden of AMR and the leading pathogen–drug combinations contributing to it is crucial to making informed and location-specific policy decisions, particularly about infection prevention and control programs, access to essential antibiotics, and research and development of new vaccines and antibiotics. There are serious data gaps in many low-income settings, emphasizing the need to expand microbiology laboratory capacity and data collection systems to improve our understanding of this important human health threat.
AMR is real, preventable, and actionable
There are immediate areas of action that we can take today to make an impact against drug-resistant infections.
Infection prevention
Preventing infections, particularly healthcare-associated infections (HAIs) that spread in hospitals, need to be considered as the first line of defense against AMR. According to the CDC, resistant bacteria cause 18% of central line-associated bloodstream infections (CLABSIs), 15% of surgical site infections (SSIs) and 10% of catheter-associated urinary tract infections (CAUTIs) in U.S. hospitals.5
- The CDC has tools available to assess infection prevention practices and guide quality improvement.
- Combatting AMR globally requires WASH (Water, Sanitation, and Hygiene) and IPC in all healthcare systems. In many low- to middle-income countries, WASH is inadequate with 1 in 3 healthcare facilities lacking hand hygiene materials at point of care and over 900 million people using healthcare facilities with no water service. Learn more about this challenge and efforts underway on the WHO, UNICEF, and WaterAid’s websites.
- The Society for Healthcare Epidemiology of America (SHEA) has updated their training course in best practices in infection prevention and control for hospital clinicians with direct patient care responsibilities. The online program, known as Prevention Course in HAI Knowledge and Control (Prevention CHKC), is currently available.
Preventing infections through vaccinations is critical for reducing the need for antibiotics. Vaccines are available for only one of the six leading global AMR pathogens, S pneumoniae. While vaccine programs are underway for several bacterial pathogens, it is also important to note that vaccines for viruses, the influenza or rotavirus vaccines, also play a role in preventing febrile illness. A reduction in febrile illness, which can lead to a reduction in antibiotic prescribing and can reduce the development of resistance. A recent study by Gupta, et.al, demonstrates that periods of high influenza activity corresponds with high rates of antibiotic resistance in respiratory and non-respiratory infections. While this study does not demonstrate causality, it does show the anecdotal link between AMR and flu season.6
Antibiotic and diagnostic stewardship
Antimicrobial stewardship programs in healthcare settings are designed to optimize antibiotic therapies, with the intention of slowing the emergence of drug-resistance. Accurate and rapid diagnostic testing is a crucial element of stewardship. Diagnostic testing can identify the infection-causing organism, determine whether it is resistant and guide the appropriate therapeutic choice. Essentially, antibiotic stewardship means being smarter—more discriminating and more appropriate—about how we (as a society) use them.
Awareness and advocacy
To change behaviors and practices around antibiotic utilization, the risk of drug resistant infections needs to better understood by organizations and individuals. Antimicrobial resistance is a complex problem that involves human health, animal management, and agriculture practices. The Antimicrobial Resistance Fighter Coalition is a is a bold collective of like-minded organizations, leaders, and individuals united in their commitment to address the threat and burden of antimicrobial resistance
Halting and reversing this massive challenge will require the combined resources and efforts of both public and private sectors. AMR has no single solution, and the challenges cannot be solved without multiple players working collectively on a common AMR agenda.
References
- Institute for Health Metrics and Evaluation. The latest estimates of global anti-microbial resistance show urgent policy action is needed to save lives. Accessed February 8, 2022. https://www.healthdata.org/news-release/ latest-estimates-global-anti-microbial-resistance-show-urgent-policy-ac.
- Centers for Disease Control and Prevention. 2019 AR threats report. Accessed February 8, 2022. https://www.cdc.gov/drugresistance/biggest-threats.html.
- Ukuhor H. The interrelationships between antimicrobial resistance, COVID-19, past, and future pandemics. J Infect Public Health. 2021;14(1):53-60.
- O’Neill J (chair). Antimicrobial resistance: tackling a crisis for the health and wealth of nations. Accessed February 8, 2022. https://amr-review.org/ sites/default/files/AMR%20Review%20Paper%20-%20Tackling%20a%20 crisis%20for%20the%20health%20and%20wealth%20of%20nations.
- Weiner LM, Fridkin SK, Aponte-Torres Z, et al. Vital Signs: Preventing Antibiotic-Resistant Infections in Hospitals — United States, 2014. MMWR Morb Mortal Wkly Rep 2016;65:235–241.
- Gupta V, Yu KC, Kabler H, Watts, et al. Antibiotic Resistance Patterns and Association With the Influenza Season in the United States: A Multicenter Evaluation Reveals Surprising Associations Between Influenza Season and Resistance in Gram-Negative Pathogens. Open Forum Infect Dis. 2022 Jan 25;9(3):ofac039. doi: 10.1093/ofid/ofac039.
Diane Flayhart, MBA, is the Global Program Leader for Antimicrobial Resistance at BD. Flayhart works to champion and support development of new Antimicrobial Resistance (AMR) program initiatives in global awareness, infection prevention/control and antimicrobial stewardship. Flayhart leads efforts for the Antimicrobial Resistance Fighter Coalition, which is mobilized by BD.
About the Author

Diane Flayhart, MBA
is the Global Program Leader for Antimicrobial Resistance at BD. Flayhart works to champion and support development of new Antimicrobial Resistance (AMR) program initiatives in global awareness, infection prevention/control and antimicrobial stewardship. Flayhart leads efforts for the Antimicrobial Resistance Fighter Coalition, which is mobilized by BD.