COVID-19 and influenza epidemics this winter?
On January 31, 2020, the Secretary of the U.S. Department of Health & Human Services (HHS) declared a Public Health Emergency followed by the declaration of a National Emergency by the President of the United States.1,2 Congress granted $25 billion to HHS to take immediate steps to prepare for the advancing COVID-19 pandemic, and soon thereafter, the National Institutes of Health (NIH) created the Rapid Acceleration of Diagnostics Initiative (RADx)3 whose task, as implied, was to accelerate the delivery of diagnostic tests to healthcare facilities and laboratories across the nation. Tremendous progress was achieved in record time, including the creation of effective vaccines, advancing the development of therapeutic agents, and the launch of new antigen and molecular diagnostic tests for the detection of SARS-CoV-2 — all in less than one year. These efforts continue with lessons learned, advancing technologies, and emerging needs.
As the pandemic spread quickly around the world, there were very few options to protect the public from widespread infection and serious disease in the beginning months. Nonpharmaceutical interventions (NPI) were introduced rapidly and promoted widely across the United States. Reduced hospitalizations and deaths were observed in locations where lockdowns, school closures, social distancing, mask-wearing, and work-from-home programs were common.4,5 This protection by NPI, although not absolute, provided HHS and partnering industries the time needed to take steps to address the emergency.
Possible linkage of nonpharmaceutical interventions to influenza
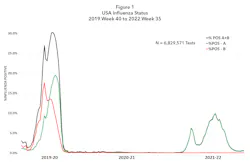
However, the impact of NPI was not limited to the spread of SARS-CoV-2. These measures also profoundly affected the incidence of other respiratory diseases, including influenza.6 Figure 1 shows the course of influenza infections in the United States from September 2019 to the present.7 At the end of the 2019–2020 season, when NPI was introduced broadly In the United States, there followed 18 months during which the influenza positivity rates rarely exceeded even 2%, as reported to the Centers for Disease Control and Prevention (CDC). Subsequently, the 2021–2022 respiratory season saw two influenza surges spanning from mid-November 2021 to April 2022. Both surges failed to achieve the higher positivity rates encountered in more “typical” influenza epidemic seasons when positivity rates often exceed 25% nationally.7
Predictions for 2022–2023
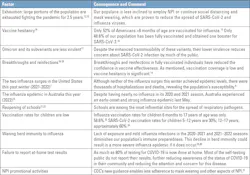
Many epidemiologists agree that a combination of both a new COVID-19 surge and a true influenza epidemic winter season in the United States is now likely. The use of NPI was likely strong enough to slow or halt this past winter’s surges, but this may not be the case this year, given the exhaustion of our populace, the low vaccination rates, the reopening of schools, the return to workplaces, the ongoing decline in NPI use, and the overall diminution of herd immunity, as discussed above.
Staying ahead through testing
The signs and symptoms for infections by SARS-CoV-2 and influenza are very similar, precluding their reliable diagnosis based on symptoms alone.28 Therefore, it seems likely that in many cases, if both COVID-19 and influenza are circulating in a community, as clearly occurred last winter, then physicians will likely want to test for all three viruses — SARS-CoV-2 and influenza (Types A and B) — at the same time.
There are currently 277 molecular and 51 rapid antigen tests with emergency use authorizations (EUAs) available for diagnosis of SARS-CoV-2 in the United States. Among these are nine multiplex molecular tests and three multiplex antigen tests for assessment of SARS-CoV-2 and influenza.29,30 Additional multiplex tests will likely receive EUAs soon. Their use of one specimen type, less hands-on time, and improved turnaround time offer advantages to laboratories, physicians, and patients — especially those who are considered high-risk and may benefit from timely therapeutic intervention.31
REFERENCES
- Determination that a public health emergency exists. Office of Sec. of Health and Humans Services. Administration for Strategic Preparedness and Response (ASPR). Published January 31, 2020. Accessed September 26, 2022. https://www.phe.gov/emergency/news/healthactions/phe/Pages/2019-nCoV.aspx.
- Declaring national emergency concerning the novel coronavirus (COVID-19) outbreak. Executive Office of the President. Published March 18, 2020. Accessed September 26, 2022. https://www.federalregister.gov/documents/2020/03/18/2020-05794/declaring-a-national-emergency-concerning-the-novel-coronavirus-disease-covid-19-outbreak.
- RADx. National Institutes of Health (NIH). Accessed September 26, 2022. https://www.nih.gov/research-training/medical-research-initiatives/radx.
- Ahlers MJ, Aralis HJ, Tang WL, et al. Non-pharmaceutical interventions and COVID-19 burden in the United States. medRxiv [Preprint]. 2021;09.26.21264142. doi: 10.1101/2021.09.26.21264142.
- 2020-2021 flu season summary. Centers for Disease Control and Prevention. Published October 25, 2021. Accessed September 26, 2022. https://www.cdc.gov/flu/season/faq-flu-season-2020-2021.htm.
- Feng L, Shang T, Wang Q, , et al. Impact of COVID-19 outbreaks and interventions on influenza in China and the United States. Nat Commun. 2021 31;12(1):3249. doi: 10.1038/s41467-021-23440-1.
- The national respiratory and enteric virus surveillance system (NREVSS). Centers for Disease Control and Prevention. Published July 14, 2022. Accessed September 26, 2022. https://www.cdc.gov/surveillance/nrevss/labs/list.html.
- Piret J, Boivin G. Viral interference between respiratory viruses. Emerg Infect Dis. 2022;28(2):273-281. doi: 10.3201/eid2802.211727.
- FluView summary ending June 11, 2022. Centers for Disease Control and Prevention. Published June 17, 2022. Accessed September 26, 2022. https://www.cdc.gov/flu/weekly/weeklyarchives2021-2022/week23.htm.
- Australian Government Department of Health. Australian influenza surveillance report – no. 11 – fortnight ending 28 August 2022. Published online 2022. Accessed September 26, 2022. https://www1.health.gov.au/internet/main/publishing.nsf/Content/ozflu-surveil-no11-22.htm.
- Milazzo A, Giles L, Parent N, et al. The impact of non-pharmaceutical interventions on COVID-19 cases in South Australia and Victoria. Aust N Z J Public Health. 2022;46(4):482-487. doi: 10.1111/1753-6405.13249.
- Crane MA, Shermock KM, Omer SB, Romley JA. Change in reported adherence to nonpharmaceutical interventions during the COVID-19 pandemic, April-November 2020. JAMA. 2021;325(9):883-885. doi:10.1001/jama.2021.0286.
- Nelson K, Lopman B. The hiatus of the handshake. Science. 2022;377(6601):33-34. doi: 10.1126/science.abp9316.
- Larson HJ, Gakidou E, Murray CJL. The vaccine-hesitant moment. N Engl J Med. 2022;7;387(1):58-65. doi: 10.1056/NEJMra2106441.
- Flu vaccination coverage, United States, 2020-21 influenza season. Centers for Disease Control and Prevention. Published October 7, 2021. Accessed September 26, 2022. https://www.cdc.gov/flu/fluvaxview/coverage-2021estimates.htm.
- Trends in number of COVID-19 vaccinations in the United States. CDC COVID Data Tracker. Published September 22, 2022. Accessed September 26, 2022. https://covid.cdc.gov/covid-data-tracker/#vaccination-trends.
- COVID-19Variants of the virus. Centers for Disease Control and Prevention. Published August 11, 2021. Accessed September 26, 2022. https://www.cdc.gov/coronavirus/2019-ncov/variants/index.html.
- Kuhlmann C, Mayer CK, Claassen M, et al. Breakthrough infections with SARS-CoV-2 omicron despite mRNA vaccine booster dose. Lancet. 2022;12;399(10325):625-626. doi: 10.1016/S0140-6736(22)00090-3.
- Hacisuleyman E, Hale C, Saito Y, et al. Vaccine breakthrough infections with SARS-CoV-2 variants. N Engl J Med. 2021;10;384(23):2212-2218. doi: 10.1056/NEJMoa2105000.
- CDC COVID-19 Vaccine Breakthrough Case Investigations Team. COVID-19 vaccine breakthrough infections reported to CDC - United States, January 1-April 30, 2021. MMWR Morb Mortal Wkly Rep. 2021;28;70(21):792-793. doi: 10.15585/mmwr.mm7021e3.
- Chao DL, Halloran ME, Longini IM Jr. School opening dates predict pandemic influenza A(H1N1) outbreaks in the United States. J Infect Dis. 2010;15;202(6):877-80. doi: 10.1086/655810.
- Mimura S, Kamigaki T, Takahashi Y, et al. Role of preschool and primary school children in epidemics of influenza A in a local community in Japan during two consecutive seasons with A(H3N2) as a predominant subtype. PLoS One. 2015; 5;10(5):e0125642. doi: 10.1371/journal.pone.0125642.
- Flu vaccination coverage, United States, 2020-21 influenza season. Centers for Disease Control and Prevention. Published October 7, 2021. Accessed September 26, 2022. https://www.cdc.gov/flu/fluvaxview/coverage-2021estimates.htm.
- COVID-19 vaccination coverage and vaccine confidence among children. Centers for Disease Control and Prevention. Published November 3, 2021. Accessed September 26, 2022. https://www.cdc.gov/vaccines/imz-managers/coverage/covidvaxview/interactive/children.html.
- Krauland MG, Galloway DD, Raviotta JM, et al. Agent-based investigation of the impact of low rates of influenza on next season influenza infections. bioRxiv. Published online 2021:2021.08.18.21262185. doi:10.1101/2021.08.18.21262185.
- Rubin R. Influenza’s unprecedented low profile during COVID-19 pandemic leaves experts wondering what this flu season has in store. JAMA. 2021;14;326(10):899-900. doi: 10.1001/jama.2021.14131.
- CDC streamlines COVID-19 guidance to help the public better protect themselves and understand their risk. Centers for Disease Control and Prevention. Published. August 11, 2022. Accessed September 26, 2022. https://www.cdc.gov/media/releases/2022/p0811-covid-guidance.html.
- Similarities and differences between flu and COVID-19. Centers for Disease Control and Prevention. January 18, 2022. Accessed September 26, 2022. https://www.cdc.gov/flu/symptoms/flu-vs-covid19.htm.
- In vitro diagnostics EUAs—Molecular diagnostic tests for SARS-CoV-2. U.S. Food and Drug Administration. Published September 22, 2022. Accessed September 26, 2022. https://www.fda.gov/medical-devices/coronavirus-disease-2019-covid-19-emergency-use-authorizations-medical-devices/in-vitro-diagnostics-euas-molecular-diagnostic-tests-sars-cov-2.
- In vitro diagnostic EUAs—Antigen diagnostic tests for SARS-CoV-2. U.S. Food and Drug Administration. Published September 6, 2022. Accessed September 26, 2022. https://www.fda.gov/medical-devices/coronavirus-disease-2019-covid-19-emergency-use-authorizations-medical-devices/in-vitro-diagnostics-euas-antigen-diagnostic-tests-sars-cov-2.
- Coronavirus (COVID-19) drugs. U.S. Food and Drug Administration. Published August 11, 2022. Accessed September 26, 2022. https://www.fda.gov/drugs/emergency-preparedness-drugs/coronavirus-covid-19-drugs.
About the Author

Sushruth K. Reddy, BS
is Associate Director of Scientific Affairs at Quidel Corporation.