Achieving equal detection for all patients in cervical cancer screening
Cervical cancer screening is undeniably one of the most successful medical screening programs ever devised. The ability to identify and treat precancerous lesions through Pap testing has led to a declining incidence in the United States over the past 50 years.1 Armed with the scientific understanding of the natural history of HPV infection and the strategic guidance of our medical communities, the goal of cervical cancer elimination seems almost attainable.
The addition of high-risk HPV (hrHPV) testing to cytologic sampling has unquestionably ushered in a new age of cervical cancer screening with their combined clinical sensitivity being superior to either Pap or hrHPV testing alone.2–7 Recently, there have been major changes to guidelines presented by various organizations in their suggested use of hrHPV testing as part of an overhaul of cervical cancer screening and management in the United States.8–10 These organizations are to be applauded for their efforts and their comprehensive evaluations. However, it remains important to critically assess their findings and conclusions to determine whether their guidance will have a meaningful impact to further reduce the burden of cervical disease in the United States.
Risk-based approach to screening
In 2019, the American Society for Colposcopy and Cervical Pathology (ASCCP) updated its management guidelines to provide greater focus on treating patients based on their risk of disease progression instead of an algorithm based solely on individual test results.8 To this end, any patient whose current test results and testing history places her risk of having a CIN3+ lesion on a biopsy at 4% or greater should be referred for colposcopic evaluation. Treating individual patient risk and not specific test results ensures that our understanding of the natural history of cervical precancer and HPV clearance rates gets incorporated into a holistic patient assessment based on all available data. The ASCCP risk calculations were developed based on a mathematical model formed from over ten years of data collected from Kaiser Permanente Northern California (KPNC).11 The population in this integrated healthcare system is generally more closely screened, resulting in lower cervical cancer rates than the broader U.S.12 Additionally, the patient demographic and socioeconomic breakdowns at KPNC are not wholly representative of the entire country.13
The new ASCCP guidelines recognize the importance of differentiating risk based on whether patients have known or unknown screening histories. However, the risk estimates for patients with poor screening history were developed using a KPNC patient’s first historical result.11 This means that the risk estimates associated with never or rarely screened groups were not developed to align with an inadequately screened population but simply a well screened population without preexisting data.
Disparities in data selection
It is not surprising, therefore, that when the KPNC risk estimations were validated for general applicability using three external data sets — namely the Centers for Disease Control and Prevention’s (CDC) National Breast and Cervical Cancer Early Detection Program (NBCCEDP), the Roche ATHENA trial and the BD Onclarity trial — it was found that all three external datasets demonstrated significantly higher immediate CIN3+ rates than KPNC. Additionally, the NBCCEDP data, which includes a greater proportion of higher risk patients, found the immediate CIN3+ rate in the poorly screened cohort to be almost three times that of the KPNC data.7
The ASCCP acknowledged that there were scenarios where risk discrepancies between the datasets would have provoked different management and changed the intended strategies in those situations. However, it should be clear that the published risk values underrepresent true risk even when compared to other well-structured clinical trials (ATHENA, Onclarity), and particularly as it relates to poorly screened patient populations (NBCCEDP). The practicing clinician should understand that the ASCCP estimated risks are not only produced by evaluation of the well screened KPNC cohort, but that those estimations remain mostly applicable to such a population.
Even accepting the KPNC risk estimates, there remain significant issues with recent guidance in cases where a clinician would come to different management decisions based on different screening strategies due to having either more or less information to assess a patient’s risk. The ASCCP accepts a primary hrHPV approach and the updated American Cancer Society (ACS) guidelines not only lay out a preference toward primary HPV screening but recommend that other methods of screening, including co-testing, be phased out of future guidelines.9 However, the KPNC and NBCCEDP data themselves demonstrate that a primary hrHPV screening strategy simply cannot accurately estimate a patient’s risk based on HPV testing alone.
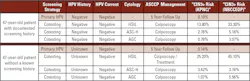
For example, a 47-year-old patient with unknown screening history who presents for initial examination and has primary hrHPV screening that is found to be negative would be estimated to have an extremely low risk of immediate CIN3+ based on ASCCP published values, and the recommended management would be for the patient to return for follow-up in five years. However, if this patient had a Pap test that demonstrated either HSIL, ASC-H, or AGC, the risks in these instances would have been deemed by ASCCP as significant enough to recommend colposcopy (Table 1).11 This is due to the high specificity of the Pap test in these categories, and highlights that risk estimation and guidance is much more accurately assessed, if not entirely dependent, on the additional information obtained through the cytology result.
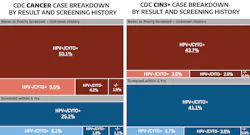
One might think that these instances of HPV negative cervical lesions constitute a small minority of CIN3+ disease overall, however, the data obtained by CDC’s NBCCEDP,7 published in support of the ASCCP, paint a starkly different picture. In the CDC data (Figure 1), 3,033 instances of CIN3+ disease were identified, and 256 of them (8.4%) occurred in patients who were entirely HPV negative. Additionally, 67 of their 359 invasive cancers (18.7%) were HPV negative as well. In 87% of the HPV negative/CIN3+ cases, and 84% of the HPV negative/cancer cases the accompanying cytology would have prompted either a shortened follow-up period or a colposcopy, given the elevated patient risk based on the additional cytology result. This finding is not unique to the NBCCEDP, and the literature now recognizes that a significant proportion of cervical disease cases test negative for HPV.3–5,14,15
While the ACS concedes that there are some co-testing screening strategies that may lead to fewer cancer cases diagnosed and fewer cancer deaths as compared to primary HPV screening,9 the authors contend that these marginal differences must be balanced against potential harms. The main harm discussed is a potential treatment-related adverse obstetric outcome. However, the cited literature associates this unquestionably concerning outcome not with the performance of cytology, or even a follow up colposcopy, but with procedures involving excisional or ablative treatment.16 Such techniques would only be necessary following an already positive biopsy obtained through colposcopy and would not be a result of utilizing cytology as a co-test to more accurately assess risk on samples already collected for HPV testing. Additionally, the safety and tolerability of colposcopy has been well established in the literature, even when performed during pregnancy.17
The ACS goes on to list physical discomfort and anxiety associated with possible additional colposcopic examinations, which would not have occurred using HPV testing alone, as a potential harm against which their mathematically modeled marginal benefit must be weighed. While it is certain that patients who had a falsely negative HPV test would not have had a colposcopy performed in the absence of an abnormal cytology result, the entire concept of a risk-based approach for referral to colposcopy ensures that only those patients with a significant enough risk of immediate CIN3+ be referred for such a procedure. By definition, the ASCCP management guidelines refer a patient to colposcopy only when the immediate risks to a patient have reached a clinical action threshold that warrants such an evaluation. The risk to the patient is what prompts a colposcopy, not a cytology result, and these thresholds have been precisely determined by the ASCCP to identify levels at which the benefits outweigh the potential discomfort and anxiety associated with its performance.
Role of co-testing
Every major guideline issuing organization recognizes that the single most important factor to the success of a cervical cancer screening program is consistent adherence to an acceptable strategy.9,18,19 Gaps in any individual testing strategy are compounded by a lack of regular attendance by the screening population. Unfortunately, while it might be convenient to utilize microsimulations from well screened populations for mathematical modeling, the reality is that the burden of this disease does not fall upon that population in the United States. It is estimated by the NIH20 that approximately one half of all cervical cancer cases occur in patients who were never screened. In the NBCCEDP data, patients with an unknown or poor screening history made up 42% of patients, yet 66% of all of the cancers were identified within this group.7
The realities of inadequate screening and their impact on various communities in the United States are not uniform. Race, ethnicity, and socioeconomic status have all been demonstrated to impact cervical cancer incidence and mortality.21–23 Clinicians who care for diverse patient populations that have limited or infrequent access to care must be aware not only of the limitations with the current guidelines and the manner in which they were developed, but the real world risks they may pose to their patients as well. It is no wonder that the ACS guidance has prompted such firm responses from the Black Women’s Health Imperative, the American Society for Clinical Pathology (ASCP) and the College of American Pathologists (CAP).24–26
Any successful screening strategy must ensure that it incorporates an understanding of the population at risk in addition to the benefits and pitfalls of any single testing strategy. The data from the NBCCEDP7 and many others3-6 continue to demonstrate that the use of cervical cytology in conjunction with hrHPV can provide an additive benefit for the identification of significant disease in HPV negative lesions. The Pap has provided us with some of the greatest successes in cancer screening in the last century and continues to be a valuable tool in the care of our patients.
While it might be tempting to dream about cervical cancer elimination in this country, the reality is much more sobering. This year, in the United States, more than 14,000 women will be diagnosed with cervical cancer and more than 4,000 will die of this preventable, screenable, and treatable disease.27 Given the resources and technological advances in cancer screening in this country, each and every one of these lost lives highlights a systemic failure. As we strive for equitable healthcare, we must first recognize the existence of distinct healthcare disparities and how they can lead to incorporation of biases into guidance. To crusade for cervical cancer eradication is to advocate for all of our patients, and specifically the underprivileged who will shoulder the burden of this disease. To win this battle, we must provide these patients with the best opportunity for disease discovery through co-testing; otherwise we are simply exacerbating existing healthcare inequities and will continue to leave them behind.
References
- Adegoke O, Kulasingam, S, Virnig B. Cervical cancer trends in the United States: a 35-year population-based analysis. J. women’s Heal. 2012;21(10): 1031–1037 (2012). doi: 10.1089/jwh.2011.3385.
- Schiffman M, et al. Relative performance of HPV and cytology components of cotesting in cervical screening. J. Natl. Cancer Inst. 2018 May 1;110(5):501-508. doi: 10.1093/jnci/djx225.
- Austin RM, Onisko A, Zhao, C. Enhanced detection of cervical cancer and precancer through use of imaged liquid-based cytology in routine cytology and HPV cotesting. Am. J. Clin. Pathol. 2018;150(5):385-392. doi: 10.1093/ajcp/aqy114.
- Kaufman HW, Alagia DP, Chen Z, Onisko A, Marshall Austin R. Contributions of liquid-based (Papanicolaou) cytology and human papillomavirus testing in cotesting for detection of cervical cancer and precancer in the United States. Am. J. Clin. Pathol. 2020;154(4):510-516. doi: 10.1093/ajcp/aqaa074.
- Vasilyeva D, Tiscornia-Wasserman P, Gonzalez A A. Negative Roche cobas HPV testing in cases of biopsy-proven invasive cervical carcinoma, compared with Hybrid Capture 2 and liquid-based cytology. J. Am. Soc. Cytopathol. Mar-Apr 2021;10(2):128-134. doi: 10.1016/j.jasc.2020.08.006.
- Zhou H, et al. Clinical performance of the Food and Drug Administration-approved high-risk HPV test for the detection of high-grade cervicovaginal lesions. Cancer Cytopathol. 2016;124(5):317-23. doi: 10.1002/cncy.21687.
- Saraiya M, et al. Risk of cervical precancer and cancer among uninsured and underserved women from 2009 to 2017. Am. J. Obstet. Gynecol. 2021;224(4):366.e1-366.e32. doi: 10.1016/j.ajog.2020.10.001.
- Perkins RB, et al. 2019 ASCCP risk-based management consensus guidelines for abnormal cervical cancer screening tests and cancer precursors. J. Low. Genit. Tract Dis. 2020 Apr;24(2):102-131. doi: 10.1097/LGT.0000000000000525.
- Fontham ETH, et al. Cervical cancer screening for individuals at average risk: 2020 guideline update from the American Cancer Society. CA. Cancer J. Clin. 2020 Sep;70(5):321-346. doi: 10.3322/caac.21628.
- Curry SJ, et al. Screening for cervical cancer US Preventive Services Task Force Recommendation Statement. JAMA. 2018 Aug 21;320(7):674-686. doi: 10.1001/jama.2018.10897.
- Egemen D, et al. Risk estimates supporting the 2019 ASCCP risk-based management consensus guidelines. J. Low. Genit. Tract Dis. 2020 Apr;24(2):132-143. doi: 10.1097/LGT.0000000000000529.
- Sung HY, et al. Papanicolaou smear history and diagnosis of invasive cervical carcinoma among members of a large prepaid health plan. Cancer 2000;88(10):2283-9.
- Katki HA, et al. Cervical cancer risk for 330,000 women undergoing concurrent HPV testing and cervical cytology in routine clinical practice at a large managed care organization. Lancet Oncol. 2011; 12(7): 663-672. doi: 10.1016/S1470-2045(11)70145-0 .
- Chen W, Chen Y. Clinical and pathological features of high-risk hpv-negative cervical cancer. Chinese Gen. Pract. (2019).
- Petry KU, Liebrich C, Luyten A, Zander M, Iftner T. Surgical staging identified false HPV-negative cases in a large series of invasive cervical cancers. Papillomavirus Res. 2017;4:85-89. doi:10.1016/j.pvr.2017.10.003.
- Kyrgiou M. et al. Adverse obstetric outcomes after local treatment for cervical preinvasive and early invasive disease according to cone depth: Systematic review and meta-analysis. BMJ 2016;354:i3633. doi: 10.1136/bmj.i3633.
- Woodrow N, et al. Abnormal cervical cytology in pregnancy: Experience of 811 cases. Aust. New Zeal. J. Obstet. Gynaecol. 1998 May;38(2):161-5. doi: 10.1111/j.1479-828x.1998.tb02992.x.
- Melnikow J, et al. Screening for cervical cancer with high-risk human papillomavirus testing updated evidence report and systematic review for the us preventive services task force. JAMA. 2018;320(7):687-705. doi: 10.1001/jama.2018.10400.
- Updated Cervical Cancer Screening Guidelines. ACOG Practice Advisory. The American College of Obstetricians and Gynecologists (ACOG), https://www.acog.org/clinical/clinical-guidance/practice-advisory/articles/2021/04/updated-cervical-cancer-screening-guidelines. Updated April 2021. Accessed October 4, 2021.
- National Institutes of Health (US). Office of Medical Applications of. NIH consensus statement. vol. 14 (National Institutes of Health, Office of Medical Applications of Research, 1996).
- National Center for Health Statistics. Recent trends in U.S. age-adjusted mortality rates, 2000-2018. US Mortality Files. https://seer.cancer.gov/explorer/application.html. Accessed October 4, 2021.
- Beavis AL, Gravitt P E, Rositch AF, Hysterectomy-corrected cervical cancer mortality rates reveal a larger racial disparity in the United States. Cancer. 2017. 123(6). doi: 10.1002/cncr.30507.
- Singh GK, Jemal A. Socioeconomic and racial/ethnic disparities in cancer mortality, incidence, and survival in the United States, 1950-2014: Over six decades of changing patterns and wdening inequalities. J. Environ. Public Health 2017; 2017:2819372. doi: 10.1155/2017/2819372 .
- College of American Pathologists. Response to ACS Letter. https://documents.cap.org/documents/cap-response-to-acs-letter.pdf. Published October 15, 2020. Accessed October 4, 2021.
- Black Women’s Health Imperative responds to American Cancer Society cervical cancer screening guidelines. Black Women’s Health Imperative. https://bwhi.org/2020/08/18/black-womens-health-imperative-responds-to-american-cancer-society-cervical-cancer-screening-guidelines/. Published August 18, 2020.Accessed September 20, 2021.
- Release of the 2020 American Cancer Society Cervical Cancer Screening Guideline. American Society for Clinical Pathology. https://www.ascp.org/content/docs/default-source/get-involved-pdfs/istp_clinical_practice_guidelines_and_resources/cetc-society-posting---acs-cervical-cancer-screening-guidelines---final-8-20-20.pdf Published 2020. Accessed September 2021.
- American Cancer Society. Key Statistics for Cervical Cancer. https://www.cancer.org/cancer/cervical-cancer/about/key-statistics.html. Accessed September 20, 2021.
About the Author

D. Yitz Goldstein, MD
serves as the Director of both the Virology and Molecular Genetic Pathology Laboratories at Montefiore Medical Center, Bronx, NY. Goldstein is an award-winning educator with a passion for evidence-based molecular diagnostic testing as a means to advance the health of the communities he serves.