The laboratory’s role in guiding best use of POCT
Continued growth in point-of-care testing (POCT) is certain as technologies improve and the benefits of POCT are realized in value-based healthcare. However, POCT is a diverse and complex area of laboratory testing, riddled with the challenges inherent to multiple locations, disparate devices, and non-laboratory trained operators. To reap the advantages POCT has to offer, POCT programs can greatly benefit from laboratory intervention and oversight. Laboratory professionals who approach POCT oversight as a team endeavor, keeping end users’ workflows and backgrounds in mind, can be instrumental in helping reap the potential benefits that POCT offers in patient care.
POCT’s renewed value instigates continued growth
The rapid turnaround time (TAT), convenience, and mobility of POCT—in specific patient scenarios—can speed clinical decision-making and treatment decisions and simultaneously help avoid other unnecessary procedures and associated risks. POCT’s rapid results can help optimize which patients receive advanced care, and improve patient understanding and engagement, giving POCT a more important role in patient-centered care.
For example, POCT can speed time to diagnosis and corresponding treatment (e.g., pregnancy test or creatinine to allow for faster imaging studies). Certain POCTs, such as pediatric influenza or a bacterial ID, have been shown to improve the appropriateness of antibiotic use. Studies have shown that reducing the TAT for cardiac marker testing from two hours to 10 minutes can decrease hospital length of stay.1 POCT lactate has been associated with reduction of mortality and ICU admissions for sepsis patients.1 Troponin and D-dimer testing have been helpful in screening for myocardial infarction (MI) and pulmonary embolism to avoid unnecessary admissions/readmissions. Overall, it is widely agreed that POCT’s ability to enable providers to make rapid decisions at the patient’s side has tremendous potential to help improve our healthcare system and the way we deliver care.
Preanalytical errors despite POCT oversight
To achieve the benefits of POCT, diagnostic accuracy, quality management, and rapid access to results are crucial. Yet, a comprehensive POCT program is extremely challenging to implement and oversee because often management is spread across multiple siloed locations. The variance in locations, operators, devices, and device capabilities, and the lack of consistency makes POCT management complex. Many laboratory professionals who oversee POCT programs are frustrated with the complexity of POCT management.
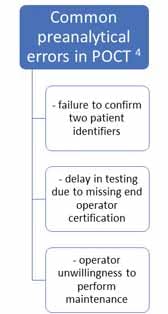
Training, ongoing certification, and proper documentation of orders and results are common challenges in POCT.2 One of the greatest areas of concern is the higher likelihood of preanalytical errors attributed to non-laboratory trained operators. Most POCT operators are from other areas in the healthcare system that often do not have a comprehensive understanding of the myriad steps that are necessary to achieve accurate lab test results; the pre-analytic, analytic, and post-analytic variables that affect quality of testing. To many, POCT pre-analytical errors appear to be outside of the laboratory’s control. Unfortunately, pre-analytical errors in POCT are quite frequent and lend to the concern about the quality of POCT results (Figure 1). Testing errors can cause delayed treatment or added costs. Whether the laboratory manages organization-wide POCT or not, poor quality POCT results reflect on the laboratory as a whole.
The highly regulated laboratory is accustomed to the multiple steps necessary to achieve high-quality standards and accurate test results. When busy end operators do not understand why they are asked to add what may seem like unnecessary steps, important details can be overlooked that can lead to erroneous results. The value of quality control (QC), quality assurance (QA), calibration, maintenance, and all of the other components necessary for accurate test results may not seem important to a healthcare worker or end operator with a non-laboratory background who is already quite busy with their other day-to-day duties. Poorly designed processes and workflows can exacerbate this problem.
Laboratorians best suited for POCT oversight
In the past, many laboratory professionals have avoided POCT oversight because of the complexity, abundance of challenges inherent to POCT, and the variables that seem to be outside of their control. These challenges added on top of an already full schedule of duties in the laboratory can feel overwhelming. However, stepping back and looking at the bigger picture is an opportune time to reevaluate POCT. From a value-based perspective of your patient population’s needs, POCT can improve patient outcomes, support population health, enhance patient engagement, eliminate risks, and/or reduce downstream spending.
Laboratory testing is “changing with the times” and POCT is going to continue to gain acceptance. Laboratory professionals are well-equipped with the knowledge base necessary to utilize POCT to its full potential. POCT requires a significant amount of support from the laboratory to ensure the quality of testing and meet regulatory requirements. Laboratorians can help determine the best selection and patient scenarios for POCT and help design workflows and processes that ensure quality results are reported and regulatory requirements are met. Including laboratory professionals as consultants in POCT selection, in addition to management, has been shown to improve the overall quality of POCT.3 POCT oversight by the laboratory improves: CLIA regulatory compliance; operator training and its documentation; review of calibrations, QC, and QA; results verification; systems for ordering, reporting, and storage of results; automated billing; and electronic
integration monitoring.4
Evaluate end user workflow
In many healthcare organizations, staff feel overworked and under constant pressure to work quickly to take care of multiple patients. This scenario can leave little patience for what seems like unnecessary steps for a simple POCT. Add to this situation a general lack of knowledge about the intricacies of laboratory testing, and you are faced with a challenge to achieve operator compliance and meet regulatory requirements.
For an effective POCT program, it behooves POC coordinators and managers to evaluate workflow with the end user in mind and look at the processes from their perspective—rather than forcing a “laboratory-oriented” protocol into a workflow that makes the process cumbersome. POCT managers can work with end users to make the workflow smooth and ensure reliable results. For instance, those who oversee POCT can apply a training system that explains the “why” behind certain steps that may seem extraneous to an end user, ensuring that training includes an understanding of the total testing process, including pre-analytical aspects and result interpretation.
For laboratory professionals to step in and make positive improvements in a POCT program, a teamwork attitude must prevail where workflows are designed with end operators in mind in a cooperative spirit. Interdepartmental teams working together can improve the POCT quality and allow the rapid TAT from POCT to achieve its clinical benefits and downstream cost savings.
REFERENCES
- St John A., Price C. P. (2018). Benefits of point-of-care testing in the Emergency Department. Acute Care Testing.
- Shaw J. L. (2016). Practical challenges related to point of care testing. Practical Laboratory Medicine (4), 22-29.
- Nichols J. (2018, August 21). The nursing-lab relationship in POCT: The good, the bad and the ugly of interdisciplinary teams. [Webinar]
- Blick K. E. (2001). The essential role of information management in point-of-care/critical care testing. Clinica Chimica Acta, 307(1-2), 159-168.
About the Author

Kim Futrell, MT (ASCP), MSHI
is the Products Marketing Manager at Orchard Software. Prior to joining Orchard in 2012, Futrell, who has a Master of Science in health informatics, worked as a lab manager for more than 20 years.