Plague take it! What’s new in viral infectious diseases?
“Plague take it!” was an expression employed by 19th and early 20th century Christians to convey anger, disgust, or frustration in a manner that would circumvent profanity.1 It simultaneously reflects the centuries-old angst and terror arising from a generational memory of plagues passed down through the centuries. But despite medical advances such as stem cell therapy, cloning, and having the total human genome at our fingertips, plagues are with us still, in ever-changing outbreaks of infectious diseases.
Highly pathogenic avian influenza virus (HPAl-H5N1)
Influenza is like “déjà vu all over again”2 and comes in more “flavors” (potential antigenic recombinants) than Baskin-Robbins ice cream. Although SARS-coronavirus-2 (SARS-CoV2) has held the lion’s share of the spotlight since late 2019, we need to remember that highly pathogenic avian influenza (HPAI-H5N1) has 16 possible expressions of hemagglutinin and 9 types of neuraminidase surface glycoproteins that could undergo antigenic shift, making it more highly transmissible and/or pathogenic. Although avian influenza viruses do not often infect humans, the amazing versatility of the agent presents a serious potential threat, and we are all too familiar with zoonotic viruses making the “leap” to humans.
In 2021–22, four humans (Ohio, Oklahoma, Colorado, and California) contracted four different antigenic variants of novel influenza. Three were found to have a swine-derived virus while one (a poultry worker in Colorado) had an avian subtype.3 To date, at least 49 million chickens and turkeys have been euthanized to try to limit the spread. However, it is already present in at least 44 states in domestic fowl and 46 states in wild birds. In many poultry husbandry facilities, birds are being kept in barns or structures with roofing to minimize the risk of transmission of highly pathogenic avian influenza (HPAI) from wild bird populations.4
Avian influenza “flies in” aboard migratory birds sweeping it from east to west across the continental United States. Influenza virus circulates and recombines to produce epidemics and pandemics due to its means of transmission and the relatively large number of potential hosts and antigenic drift and shift. We need full cooperation and communication among diagnostic laboratories, immunization sites/programs, domestic poultry producers, the U.S. Department of Agriculture, and the Centers for Disease Control and Prevention (CDC) to keep a watchful eye on this potential threat.
The 2022–23 egg-derived vaccine was developed against the following: an A/Victoria/2570/2019 (H1N1)pdm09-like virus; an A/Darwin/9/2021 (H3N2)-like virus; a B/Austria/1359417/2021-like virus (B/Victoria lineage) and a B/Austria/1359417/2021-like virus (B/Victoria lineage); and a B/Phuket/3073/2013-like virus (B/Yamagata lineage).3
Monkeypox virus
Monkeypox (mpox) viral infections in humans in Africa were first recognized in 1970. However, 2022 saw it skyrocket to World Health Organization (WHO) global emergency status.6
At that time, only circulating vaccine-derived oral poliovirus (cVDPV) and COVID had achieved that status.7 The first case in the United States was in a man from Texas who had just returned from Nigeria via Mexico.8
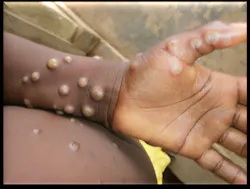
Following an incubation period of 5–21 days, symptoms develop including exhaustion, fever, muscle or back aches, swollen lymph nodes, and chills. Painful dermal lesions progress from papule to pustule finally ending in crusted sores. Lesions do not always spread to many areas of the body and the patient may display a few lesions or only one. According to the CDC, lesions frequently occur “in the genital/anogenital regions or in the mouth. In some patients, monkeypox symptoms include rectal bleeding, pain, and purulent or bloody stools.”9 According to research published in the New England Journal of Medicine, “Transmission was suspected to have occurred through sexual activity in 95% of gay or bisexual men with the infection.”9
It should be noted that anyone can contract this infection via skin-to-skin contact or by contact with contaminated towels, surfaces, or inanimate objects.10 In Brazil, a nurse contracted the virus from a patient via a needlestick procedure while attempting to obtain a specimen from a lesion for confirmation by laboratory professionals.10 According to the CDC, needles or other “sharps” should never be used to collect specimens from suspected mpox patients. CDC describes in detail what PPE are advised when working with mpox patients and specimens.
Worldometer data as of November 4, 2022, reflect that there have been 78,229 cases of monkeypox and six deaths caused by the virus. Vaccines (Jynneos and ACAM2000) against monkeypox are currently being stockpiled by the federal government in quantities sufficient for vaccinating millions of Americans against monkeypox.11,12
Ebolavirus disease
Ebolavirus disease (EVD), formerly known as Ebola Hemorrhagic Fever, is a rare but extremely severe viral infection with a complex clinical course. The mortality rate ranges from 70–90%.13,14 It has caused the deaths of thousands of residents of the Democratic Republic of Congo (DRC), Sierra Leone, Liberia, Gabon, and countries in central and west Africa in about 40 outbreaks since it was discovered in 1976 simultaneously in Nzara, South Sudan and in Yambuku, DRC.13
EVD interferes with coagulation, which often gives way to both internal and external bleeding. Other symptoms include fever, headache, muscle pain, sore throat, rash, vomiting, and diarrhea. Severe dehydration potentiates the mortality rate.15 It is characterized by bleeding from every orifice of the body and formation of bullous skin lesions filled with blood. EVD is a sylvatic, zoonotic virus and humans contract it from fruit bats, small antelopes, primates, and numerous animals bagged as “bush meat,” which is highly prized, although the capture and consumption of bush meat is illegal for obvious health reasons.
The most recent outbreak of EVD occurred in a man from Uganda who presented with fever and bleeding from the eyes on September 11, 2022. Over the next four days, his condition worsened with muscle aches and bloody diarrhea. EVD caused by the Sudan virus (one of five subtypes of Ebola virus) was confirmed by PCR, and he died on September 19, 2022. By October 26, 2022, there had been a total of 115 confirmed and 21 probable cases of Ebola Sudan virus infection with 32 confirmed and 21 probable deaths. The case fatality ration among confirmed cases was 27.8%.16
EVD can be diagnosed by antibody-capture, enzyme-linked immunosorbent assay (ELISA), antigen-capture tests, serum neutralization, reverse transcriptase polymerase chain reaction (RT-PCR), electron microcopy, and virus isolation in cell culture.17,18
On October 6, 2022, the United States announced that travelers from Uganda would be screened for EVD at one of five U.S. major airports. These include JFK (NY), Washington-Dulles (VA), Newark Liberty (NJ), Chicago-O’Hare (IL), and Hartsfield-Jackson Atlanta (GA).19
Circulating vaccine-derived poliovirus
On September 13, 2022, the CDC confirmed that circulating vaccine-derived poliovirus (cVDPV2) (antigenically similar to Sabin-like 2 virus) is in the Rockland and surrounding counties in New York. A case of paralytic polio was detected in an unvaccinated adult, and the virus was present in several samples of wastewater from the same location. Additionally, cVDPV2 has also been found in wastewater samples from the Jerusalem district in Israel and in London and Ireland indicating community transmission.20 This is a sobering fact because the wild type was eliminated from the United States in 1979 thanks to vaccine diligence.
Two failures enabled the re-emergence of this virus: 1. failure to adhere to good health practices by ignoring polio vaccination and 2. the instability of the RNA polioviruses that are used in live, attenuated vaccines and their tendency to back-mutate in nature and regain enough of the original pathogenicity to induce illness (and more rarely, paralysis). Live attenuated oral poliovirus vaccine is still given in many countries due to its ease of use, low economic impact, and efficiency in halting outbreaks.
As Saint Francis de Sales (1091–1153) reportedly stated, “The road to Hell is paved with good intentions.”21 Those of us who knew the threat of polio before killed injectable vaccine or live attenuated polio vaccine were available are particularly frustrated. Senior laboratory professionals will remember the tragic photos of dozens of children in “iron lung” devices that prevented them from dying of asphyxiation following a paralytic course of poliovirus infection. Even children who seem to fully recover can develop new muscle pain, weakness, or paralysis as adults, 15 to 40 years later. This is called post-polio syndrome.22
Poliovirus is highly contagious and readily spreads via person-to-person contact. It can be detected in a patient’s throat and intestinal tract, illustrating that it is transmitted by a fecal-oral route. Coughs and sneezes by an infected individual can also spread the virus, although less efficiently. Unfortunately, poliovirus can be spread by asymptomatic persons.
Inactivated poliovirus vaccine (IPV) is administered via injection, and this type of vaccine has been used in the United States since 2000. Oral polio vaccine (OPV) is still used throughout much of the world.22
Parechovirus
From April to May 2022, 23 infants aged 5 days to 6 months were admitted to the Monroe Carell Jr. Children’s Hospital at Vanderbilt University in Nashville, TN with parechovirus (PeV) infection.23 Twenty-one of these infants recovered without residual health issues, but one was left at risk for blood clots and hearing deficits.24 Another young patient was at serious risk for developmental delays and had experienced persistent seizures.
This comprised an “unusually large cluster” and the CDC determined that the PeV involved was circulating on a nationwide basis since May 2022. The virus is so common that doctors suggested that PeV be considered in infants with seizures and fever. Very little distinguishes it from common rhinovirus infections other than its intensity.23,24 PeV is dangerous in newborns, but causes milder symptoms that often go undiagnosed in older kids and adults.
Respiratory syncytial virus
In Memphis, Tennessee at Le Bonheur Children’s Hospital, cases of respiratory syncytial virus (RSV) are skyrocketing in pediatric patients this fall. By October 27, there were no beds left in the pediatric intensive care (ICU) unit. The vast majority of these children were suffering from RSV or influenza. The hospital reported 290 admissions due to respiratory viruses in September, and in November, influenza was on the rise, with 8–10 admissions daily due to either influenza or RSV. The emergency department averaged about 50 admissions per day due to RSV or influenza and 187 resulting from asthma.25
RSV can cause illness in persons of any age, but it presents the greatest risk of life to premature infants and those with pulmonary pathology due to a variety of elements. It causes damage in the bronchioles where large syncytial cells form containing multiple nuclei. The result is “plugging or occlusion of bronchiolar airway lumens by sloughed necrotic and irregular epithelium, combined with peribronchiolar infiltration and submucosal edema.”26 In adult and older pediatric patients, RSV can cause mild cold-like symptoms, including congested or runny noses, low-grade fever, sore throat, sneezing, and headache.
Severely affected infants exhibit gasping, shallow and slow breathing, coughing, poor feeding, and unusual tiredness and irritability.25,26 High-risk patients can be treated with Synagis, which is an RSV F protein inhibitor monoclonal antibody. It is not a vaccine but can be administered to high-risk pediatric patients by injection at monthly intervals throughout the peak RSV season.27
Conclusion
Our battle with viruses is very old and is yet almost completely new when one considers the late trend in emerging agents. We need to be very watchful of zoonotic agents that have “jumped” from various animals to infect humans. The SARS group of viruses arose from pangolins (scaly anteaters, bats, etc.), HIV (chimpanzees), EBV (fruit bats, primates, etc.), avian influenza (migratory birds), and monkeypox (monkeys, sylvan rodents, etc.). These have caused major health disasters, and we have not even gotten into rabies (mammals), Hantavirus (rodents), and Nipah virus (fruit bats).
Emerging virus “sentinel” labs and medical facilities around the world, in conjunction with the CDC, WHO, ProMed, Epicore, the National Institutes for Health (NIH), and the International Society for Infectious Diseases (ISID), continually monitor and produce reports about “new” viruses. We can never be too careful. As the anonymous saying goes, “What doesn’t kill you mutates and tries again.”
REFERENCES
- Peirce J, McMillan A, eds. Plague Take It: A COVID Almanac by and about Elders. Loose Cannon Press; 2021.
- Knapel R. Yogi Berra: “it’s Deja vu all over again” and his 25 greatest quotes. Bleacher Report. Published April 7, 2011. Accessed November 23, 2022. https://bleacherreport.com/articles/657044-yogi-berra-its-deja-vu-all-over-again-and-his-25-greatest-quotes.
- Merced-Morales A, Daly P, Abd Elal AI, Ajayi N, et al. Influenza Activity and Composition of the 2022-23 Influenza Vaccine - United States, 2021-22 Season. MMWR Morb Mortal Wkly Rep. 2022;22;71(29):913-919. doi: 10.15585/mmwr.mm7129a1.
- Usda Aphis. Usda.gov. Published July 20, 2022. Accessed November 23, 2022. https://www.aphis.usda.gov/aphis/ourfocus/animalhealth/animal-disease-information/avian/avian-influenza/hpai-2022/2022-hpai-commercial-backyard-flocks.
- Paisley A. 5 things to know about monkeypox. ONE. Published July 28, 2022. Accessed November 23, 2022. https://www.one.org/international/blog/facts-myths-monkeypox-outbreak/.
- HAN archive - 00466. Cdc.gov. Published May 20, 2022. Accessed November 23, 2022. https://emergency.cdc.gov/han/2022/han00466.asp.
- CDC. Clinical recognition. Centers for Disease Control and Prevention. Published November 21, 2022. Accessed November 23, 2022. https://www.cdc.gov/poxvirus/monkeypox/clinicians/clinical-recognition.html.
- Traveler hospitalized in Dallas with case of human monkeypox, CDC says. ABC13 Houston. Published July 16, 2021. Accessed November 23, 2022. https://abc13.com/human-monkeypox-in-texas-dallas-case-cdc-person-gets-on-flight-to/10892077/.
- Thornhill JP, Barkati S, Walmsley S, et al. Monkeypox Virus Infection in Humans across 16 Countries - April-June 2022. N Engl J Med. 2022;25;387(8):749-750. doi: 10.1056/NEJMoa2207323.
- Carvalho LB, Casadio LVB, Polly M, et al. Monkeypox Virus Transmission to Healthcare Worker through Needlestick Injury, Brazil. Emerg Infect Dis. 2022;28(11):2334-2336. doi: 10.3201/eid2811.221323.
- Information for healthcare professionals. Cdc.gov. Published November 21, 2022. Accessed November 23, 2022. https://www.cdc.gov/poxvirus/monkeypox/clinicians/.
- Assistant Secretary for Public Affairs (ASPA). HHS orders 2.5 million more doses of JYNNEOS vaccine for Monkeypox preparedness. US Department of Health and Human Services. Published July 1, 2022. Accessed November 23, 2022. https://www.hhs.gov/about/news/2022/07/01/hhs-orders-2-point-5-million-more-doses-jynneos-vaccine-for-monkeypox-preparedness.html.
- Ebola virus disease. World Health Organization. Published February 23, 2021. Accessed November 23, 2022. https://www.who.int/en/news-room/fact-sheets/detail/ebola-virus-disease. https://www.cfr.org/backgrounder/what-ebola-virus.
- Klobucista C, Renwick D. What is the Ebola virus? Council on Foreign Relations. Published October 23, 2014. Accessed November 28, 2022. https://www.cfr.org/backgrounder/what-ebola-virus?
- Uganda Ebola outbreak, September 2022. Cdc.gov. Published November 23, 2022. Accessed November 29, 2022. https://www.cdc.gov/vhf/ebola/outbreaks/uganda/2022-sep.html.
- Ebola disease caused by Ebola Sudan virus – Uganda. World Health Organization (WHO). Published October 28, 2022. Accessed November 28, 2022. https://www.who.int/emergencies/disease-outbreak-news/item/2022-DON421.
- Diagnosis of Ebola virus disease. Centers for Disease Control and Prevention (CDC), Published October 14, 2022. Accessed November 28, 2022. https://www.cdc.gov/vhf/ebola/diagnosis/index.html#:~:text=Ebola%20virus%20can%20be%20detected,low%20levels%20of%20Ebola%20virus.
- 5., Kebenei CK, Okoth P. Ebola virus disease, diagnostics and therapeutics: Where is the consensus in over three decades of clinical research? Scientific African. 2021;13(e00862):e00862. doi:10.1016/j.sciaf.2021.e00862.
- Screening patients. Cdc.gov. Published October 27, 2022. Accessed November 23, 2022. https://www.cdc.gov/vhf/ebola/clinicians/evaluating-patients/index.html.
- United States confirmed as country with circulating vaccine-derived poliovirus. CDC. Published September 13, 2022. Accessed November 23, 2022. https://www.cdc.gov/media/releases/2022/s0913-polio.html.
- The road to hell is paved with good intentions. GRAMMARIST. Published January 13, 2019. Accessed November 23, 2022. https://grammarist.com/proverb/the-road-to-hell-is-paved-with-good-intentions/.
- CDC. What is polio? Centers for Disease Control and Prevention. Published August 12, 2022. Accessed November 23, 2022. https://www.cdc.gov/polio/what-is-polio/index.htm.
- Traub A. Parechovirus sickened 23 infants in Nashville, C.d.c. says. The New York times. Published July 29, 2022. Accessed November 23, 2022. https://www.nytimes.com/2022/07/29/science/parechovirus-nashville-infants-children.html.
- Tao L, Fill MA, Banerjee R, Humphries RM. Notes from the Field: Cluster of Parechovirus Central Nervous System Infections in Young Infants - Tennessee, 2022. MMWR Morb Mortal Wkly Rep. 2022;29;71(30):977-978. doi: 10.15585/mmwr.mm7130a5.
- Hrach M. No ICU beds open at Le Bonheur amid RSV and flu cases. FOX13 News Memphis. Published October 27, 2022. Accessed November 29, 2022. https://www.fox13memphis.com/news/local/flu-rsv-cases-flowing-into-le-bonheur-childrens-hospital/A3QKUXDHWFAVBGFUTRLYO3QXJ4/.
- Pickles RJ, DeVincenzo JP. Respiratory syncytial virus (RSV) and its propensity for causing bronchiolitis: Pathology of RSV bronchiolitis. J Pathol. 2015;235(2):266-276. doi:10.1002/path.4462.
- HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use SYNAGIS safely and effectively. See full prescribing information for SYNAGIS. SYNAGIS (palivizumab) injection, for intramuscular use Initial U.S. Approval: 1998. Synagis.com. Accessed November 23, 2022. https://www.synagis.com/synagis.pdf.
About the Author

Linda L. Williford Pifer PhD, SM(ASCP), GS(ABB)
is Professor of Diagnostic and Health Sciences at the University of Tennessee Health Science Center and established the diagnostic virology lab at Le Bonheur Children’s Hospital, Memphis, TN.