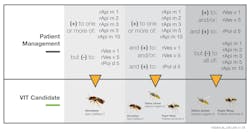
Component testing emerging as critical indicator for anaphylactic risk
Earning CEUs
For a printable version of the July CE test go HERE or to take test online go HERE. For more information, visit the Continuing Education tab.
LEARNING OBJECTIVES
Upon completion of this article, the reader will be able to:
1. Recall the causes and symptoms of anaphylaxis response in humans.
2. Recall the types of allergic sensitivities that most commonly are involved in an anaphylaxis response.
3. Discuss specific IgE blood tests on the market today and the types of allergic sensitivities they identify.
4. Discuss how the specific IgE blood tests help healthcare practitioners make informed decisions about their patients’ allergy management plans.
Most allergic reactions elicit mild to moderate symptoms, such as sneezing, watery eyes, or a rash. Sometimes, though, the immune system overreacts to an allergen, creating a serious, life-threatening condition called anaphylaxis. During anaphylaxis, a person can experience an almost instantaneous rush of symptoms, which may include a rash (typically hives), a high pulse, and even shock (called anaphylactic shock). An anaphylactic reaction like this needs to be treated immediately with an epinephrine (adrenaline) injection; without immediate treatment, anaphylaxis can be fatal.
What causes anaphylaxis?
Researchers estimate that between 1.6 percent and 5.1 percent of Americans have experienced anaphylaxis.1 In many cases, medications are to blame. However, anaphylaxis can also be caused by other more ordinary occurrences, such as being stung by an insect or by eating foods that are known to cause allergies, such as peanuts or tree nuts. Studies have shown that food-related anaphylaxis is relatively common, although fatalities remain rare with a reported range of approximately 0.03 to 0.3 deaths per million person years in the general population.2
Likewise, stinging insect allergy is fairly prevalent, affecting up to 5 percent of the population during their lifetime,6 and one of the most frequently associated with anaphylaxis in both adults and children.12 Anaphylaxis to insect stings has occurred in 3 percent of adults and can be fatal even on the first reaction,3 and researchers estimate that there are between 90 to 100 deaths per year caused by insect sting anaphylaxis.4
At a molecular level within the body, anaphylaxis is the result of a rapid and complex series of chemical reactions, some of which remain poorly understood, in part because they can be quite individualistic. For example, people who have experienced an allergic reaction to an insect sting have a 60 percent chance of a similar or worse reaction if stung again.4 That is why new diagnostics that gauge a patient’s sensitization to certain proteins can play a critical role in helping clinicians determine who is most at risk of anaphylaxis.
The recent evolution of allergy testing
Historically, standard clinical management for allergies involved an assessment of a patient’s symptoms and history, followed by skin prick testing and/or immunoassays of specific whole allergen immunoglobulin E (IgE). But the emerging field of molecular allergology is changing all that with innovative, enhanced methods that help healthcare providers refine the diagnosis and treatment of allergies.
Today, a routine blood test coupled with advanced diagnostics can allow healthcare providers to identify, on a molecular level and with great specificity, which component proteins a patient is sensitized to. These new specific IgE blood tests, which are also called component tests, quantify IgE antibodies to single, pure allergen components, and they can be used to help pinpoint the cause of an allergy. In addition, these tests can help gauge where a patient falls on the spectrum of possible reactions – and identify who is most at risk of anaphylaxis.
Specific IgE component blood tests enable more proactive allergy diagnosis and management and are now available to identify allergic sensitization to:
- environmental allergens, including seasonal and perennial triggers, both outdoor and indoor
- common food allergens, such as peanut, tree nut, egg, and milk
- pet allergens, including dog, cat, and horse
- stinging insect allergens, including up to eight different proteins found in the venom of bees and wasps
It is also important to note here that specific IgE component blood tests, which are available in most major U.S. laboratories, can be ordered for patients of any age, regardless of skin condition, current medication, disease activity or pregnancy status. Since patients often react to more than one allergen, they can also be quite helpful for distinguishing primary allergic sensitization from cross reactivity. Cross-reactivity occurs when the proteins in one substance (e.g., pollen) are similar to the proteins in another (e.g., fruit and vegetables). Then, when a patient with an allergy to one protein comes in contact with a similar protein, their immune system can react in the same way, even though they may not be truly allergic to the similar protein.
Specific IgE blood tests should be ordered with reflex
Clearly, results from specific IgE blood tests can have significant diagnostic implications. The fastest, easiest way to get these results is for healthcare professionals to order specific IgE blood tests with reflex. That way, if the initial testing results to a whole allergen test falls outside of the normal range, an additional test – the reflex to component specific IgE blood tests – will be performed to gather additional information to aid in a proper diagnosis. Because the reflex test happens automatically, the patient does not have to go back to the lab for a second blood draw. That saves the patient time and potential pain.
On the downside, reflex testing does involve additional expense, although the cost is not exorbitant. Remember, reflex testing only occurs if a whole allergen test indicates sensitization, and as a proxy for what an insured patient could reasonably expect to be billed, the Centers for Medicare & Medicaid Services (CMS) reimburses $22.14 per component allergen.Allergy component testing helps improve the diagnosis of peanut allergy
Among all the possible food allergies, allergen component testing has been the most extensively studied for the diagnosis of peanut allergy – and for good reason. Peanut allergic reactions are generally the most common culprit of fatal food-induced anaphylaxis, with the highest-risk groups being adolescents with asthma.13 In fact, studies show that people allergic to peanuts have a higher risk of anaphylaxis compared with people who are allergic to other foods, like milk or egg.13 In addition to all that, peanuts and peanut products are quite commonplace, making it especially difficult to manage the loss of safety and spontaneity that comes with a peanut allergy diagnosis.
Diagnostic testing for peanut allergy typically starts with blood or skin testing for the whole allergen, i.e., all of the proteins found in a peanut; however, once these tests produce a positive result showing that a patient is sensitized to peanuts, the next questions become, “Is this patient at risk for a systemic reaction like anaphylaxis, or can they actually tolerate peanuts, and therefore be a good candidate to proceed with an oral food challenge?”
Specific IgE component blood tests can help provide those answers. To better diagnose peanut allergies, component blood testing can assess sensitization to several peanut proteins, including Ara h 1, Ara h 2, Ara h 3, Ara h 6, Ara h 8, and Ara h 9. Sensitization to Ara h 1, 2, 3, and 6 indicates a higher likelihood of having a systemic reaction to peanuts.14 Sensitization to Ara h 8 is mainly associated with either no clinical reactivity or with isolated local reactions, for example, oral allergy syndrome.15
These specific IgE blood tests enable labs to provide a more complete view of a patient’s overall peanut sensitization, including whether a patient is at risk for cross-reactivity. The results can play a critical role in understanding the likelihood of a life-threatening reaction, and help clinicians make more informed decisions regarding their patients’ allergy management plans.Allergy component testing improves diagnosis of tree nut allergy
Tree nut allergies are another common type of food allergy for both children and adults. Tree nuts come in a wide range of varieties, including almonds, cashews, and walnuts, to name just as few. As with the allergic reactions to peanuts described above, tree nut allergic reactions can run the gamut – from less severe, localized reactions, such as itching and tingling of the mouth and lips, to widespread, systemic reactions, including anaphylaxis. Where someone falls on this spectrum of reactions may depend on which protein in different tree nuts is causing the reaction, and knowing which protein is causing the reaction is important because different proteins can cause different allergic reactions.
Specific IgE blood testing is currently available for tree nut components of hazelnuts, walnuts, brazil nuts, and cashews. That means that component testing can help healthcare providers refine the diagnosis to determine if a patient is allergic to one tree nut or more than one and assess the likelihood of a systemic reaction such as anaphylaxis. As with specific IgE testing for peanut allergies, testing with allergen components specific to tree nuts can help healthcare providers determine when to recommend oral food challenges.
Allergy component testing helps improve the diagnosis of allergies to venom from stinging insects.
Allergies to the venom of stinging insects are also fairly prevalent, and in some cases, may result in severe allergic reactions, including anaphylaxis. Over 16.5 million Americans have a history of systemic anaphylactic reactions to insect stings,6 and researchers estimate that between 90 to 100 deaths per year are caused by insect-sting anaphylaxis.4 The insects involved are from the Hymenoptera order and include bees, wasps, hornets, yellow jackets, and fire ants – all of which release venom when they sting.
Recently, the U.S. Food and Drug Administration (FDA) approved diagnostic specific IgE blood testing for a number of allergenic components associated with honeybees and wasps. To facilitate an even more precise diagnosis, several honeybee and wasp allergens have been precisely characterized and are now available as recombinant antigens for component-resolved diagnostics. Results from these specific IgE tests with component-resolved diagnostics can help specialists and other healthcare providers discriminate between true sensitization and cross reactivity. They can also help identify culprit insect(s) in patients with inconclusive patient history and guide the selection of future therapy, including prescription of venom immunotherapy.
Here are just two examples to illustrate the point: 68 percent of patients with a history of reactions to honeybee venom are sensitized to protein components Api m 3 or Api m 10, and 4.8 percent are sensitized to these components exclusively.7 However, because these allergen components are under-represented or absent from some of the licensed preparations used for honeybee venom immunotherapy, patients with Api m 3 or Api m 10 sensitivity exclusively may not always be getting the treatment that is most effective for them.7
Similarly, up to 50 percent of venom allergic patients test positive for both bee and wasp venom.8 For them, specific IgE blood testing with recombinant protein allergens rApi m 1, rVes v 1, and rVes v 5 can discriminate double sensitization from cross reactions and nonspecific sensitization related to carbohydrate determinants frequently found in Hymenoptera venom.16 As these examples show, specific IgE tests with component-resolved diagnostics using recombinant venom allergens can improve the specificity of results, leading to more successful venom immunotherapy.
Research on allergies to venom from stinging insects has also revealed that tryptase tests can aid in the diagnosis of other medical conditions. More specifically, researchers have learned that mastocytosis occurs in approximately 2 percent of patients with insect sting allergy, and that insect sting allergy occurs in approximately 25 percent of patients with mastocytosis.9 Mastocytosis is a condition that occurs when mast cells, which play a fundamental role in immune responses, accumulate in skin and/or internal organs.
Studies indicate that mast cell activation may also initiate certain allergic reactions, although the exact mechanism remains unclear. Because a severe insect sting reaction may be the first symptom of mastocytosis, some experts recommend that patients with severe reactions be evaluated for mastocytosis.10 For people with diagnosed mastocytosis, experts recommend testing for Hymenoptera venom sensitivy, and testing basal serum tryptase for patients who have had a systemic reaction to an insect sting or before starting venom immunotherapy.9
Improved testing means better allergy risk management
If someone’s immune system overreacts to an allergen, the serious, life-threatening condition called anaphylaxis can result. Given that 30 percent of adults and 40 percent of children in the U.S. suffer from allergies – and that those percentages are continuing to climb – it is growing increasingly critical to be able to assess which allergy sufferers are at the greatest risk of anaphylaxis.11
Fortunately, scientists have developed a new generation of advanced diagnostics that can precisely identify, at the molecular level, specific proteins a patient is sensitized to. These new specific IgE allergen component blood tests, are now available for many of the most common allergic triggers, including food allergens, pet allergens, and stinging insect allergens. The tests work by quantifying IgE antibodies to single, pure allergen components, based on clinical studies. They have been designed to help identify the allergic sensitizations and help clarify the options for effective allergy management. Specific IgE blood tests can also help gauge where a patient falls on the spectrum of possible allergic reactions, ranging from a local reaction such as oral itching to a systemic reaction during anaphylaxis.
Once identified, those at risk of anaphylaxis need to take precautions. First and foremost, they need to avoid coming into contact with their allergic triggers. However, since that is not always possible, someone who is at risk for anaphylaxis, should always carry auto-injectable epinephrine and learn how and when to self-administer it. The hormone epinephrine (also known as adrenalin) can reverse the symptoms of anaphylaxis, for example, raising blood pressure, increasing heart rate, and opening constricted airways to improve breathing.
But epinephrine is a rescue medication only, and anyone who has had a severe allergic reaction still needs to be seen immediately by a medical professional. Because anaphylaxis is so serious and can be life-threatening, many people who are at risk of it also wear a bracelet or necklace that alerts others of their allergies. That way, in an emergency, caregivers or medical professionals are able to administer the appropriate treatments as quickly as possible.
Assessing someone’s risk of anaphylaxis is enormously beneficial. On the one hand, learning that they are at low risk can ease a patient’s mind; on the other, learning that they are at high risk can help a patient take the proper precautions. Combining specific IgE allergen component blood tests with whole allergen testing and a comprehensive clinical history allows specialists and other healthcare providers to better assess their patients’ sensitizations to common allergens. This comprehensive approach allows clinicians to identify allergy triggers more precisely. Then, they can discriminate between true sensitization and cross reactivity, determine where a patient falls on the spectrum of possible allergic reactions, and create optimal allergy management protocols.
References:
- Wood RA et al. Anaphylaxis in America: The Prevalence and Characteristics of Anaphylaxis in the United States. J Allergy and Clin Immunol. 2014; 133(2):461-7.
- Turner PJ et al. Fatal Anaphylaxis: Mortality Rate and Risk Factors. J Allergy and Clin Immunol Pract 2017; 5(5):1169-1178.
- Golden DB. Insect Sting Anaphylaxis. Immunol Allergy Clin of North AM.2007; 27(2):261-vii.
- Insect Sting Allergy. ACAAI. https://acaai.org/allergies/types/insect-sting-allergy
- Scurlock AM, Burks WA. Peanut Allergenicity. Ann Allergy Asthma Immunol. 2004 93 (5 Suppl 3): S12–8.
- Ludman, Sian W, and Robert J Boyle. “Stinging Insect Allergy: Current Perspectives on Venom Immunotherapy.” J Asthma Allergy. 2015; 8:75-86.
- Kohler J et al. Component Resolution Reveals Additional Major Allergens in Patients with Honeybee Venom Allergy. J Allergy and Clin Immunol. 2014; 33(5): 1383–1389.
- Jakob T et al. Diagnostics in Hymenoptera Venom Allergy: Current Concepts and Developments with Special Focus on Molecular Allergy Diagnostics. Allergo J Int. 2017;26(3):93–105.
- Golden DB, et al. Stinging insect hypersensitivity: A practice parameter update 2016. Ann Allergy Asthma and Immunol. 2017;118(1):28–54.
- Sahiner UM, Durham SR. Hymenoptera Venom Allergy: How Does Venom Immunotherapy Prevent Anaphylaxis from Bee and Wasp Stings? Front in Immunol. 2019; 10:1959.
- Allergy Statistics and Allergy Facts. WebMD. www.webmd.com/allergies/allergy-statistics.
- Food Allergy. ACAAI. https://acaai.org/allergies/types/food-allergy.
- Peanut Allergy: Common Symptoms and Causes. Allergy Insider. Thermo Fisher. https://www.thermofisher.com/diagnostic-education/patient/us/en/allergy-types/food-allergies/peanut-allergy.html
- Namork, E, Stensby BA. Peanut Sensitization Pattern in Norwegian Children and Adults with Specific IgE to Peanut Show Age-Related Differences. Allergy Asthma Clin Immunol. 2015; 11 (32).
- Asarnoj A et al. Peanut Component Ara h 8 Sensitization and Tolerance to Peanut. J Allergy and Clin Immunol. 2012; 130(2) 468–472.
- Müller U et al. IgE to recombinant allergens Api m 1, Ves v 1, and Ves v 5 distinguish double sensitization from cross reaction in venom allergy. Allergy. 2012; 67:1069–1073.
About the Author

Dr. Lakiea Wright
serves as Medical Director of U.S. Clinical Affairs at Thermo Fisher Scientific-ImmunoDiagnostics.