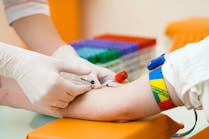
The blood-sample collection is widely considered the most fundamental of procedures in the laboratory setting, remarkable both for its simplicity and its frequency. We collect blood samples from patients for hematology or chemistry testing, and we do it billions of times each year. In terms of both the equipment and the time involved, blood-sample collection continues to be a major focus of laboratory activity and a critical, if often overlooked, area of responsibility for nursing, phlebotomy and laboratory teams.
In light of the scope of activity in blood-sample collection, even minor improvements in product design that reduce risks or improve efficiency are positioned to have a significant impact on laboratory costs, patient experience and both patient and healthcare-worker safety. This is especially true when collecting blood samples from patients with difficult venous access (DVA), where the blood flow is compromised due to low pressure or narrow vessel diameter, making it difficult or impossible to collect a sufficient blood sample. DVA is a common condition that affects thousands of infants, children, and seniors as well as many patients with cancer, diabetes, chronic kidney disease, and other illnesses. In DVA patients, the products and procedures widely used in blood collection often are unable to produce an adequate sample, while the collection process itself can present a risk of damage to venous tissue, vein collapse, and other health problems for patients. The need for repeated attempts to collect blood also increases the risk of iatrogenic anemia in patients, as well as risk of transmission of bloodborne pathogens to nurses and phlebotomists.
Strategies in blood-sample collection continue to be based in general terms on three options, each with its own risks, benefits, and technological support:
Venous blood collection: Venous blood is the optimal target for most blood sampling, and the prevailing technological options for blood collection ar needles or blood-collection sets (also known as wingsets). In recent years, advances in needle-safety technology have significantly reduced the risk of needlestick injuries. In first-generation technology, the needle-safety feature is manually activated after collection. Advances in technology then led to a safety feature that could be activated while the needle is inserted in the vein. More recently, needle technology allows passive activation of the safety feature as soon as the blood collection is initiated.
Despite these advances, the use of a needle to access blood for sampling requires both a level of skill and some special considerations in patient and healthcare-worker safety, especially in treatment involving DVA patients. As a general rule, nurses or phlebotomists who are more experienced in blood collection will be better able to complete a safe and successful first-attempt blood collection using a needle. Even among experienced blood-draw professionals, however, the use of a needle presents a potential risk of hematoma, thrombus, or damage to blood cells that can compromise sample analysis.
The use of a blood-collection wingset can address some of these issues. Many healthcare workers, particularly nurses, consider wingsets more user-friendly because the wings allow easier insertion of the needle into the vein, and the presence of tubing makes it easier to manipulate a holder and blood-collection tube with minimal effect on the patient. When the blood-collection tube is pushed onto the needle present in the holder, the presence of tubing diffuses this force, thus minimizing the movement of the needle in the vein and reducing the risk of damage to the venous tissue.
Line or catheter-based blood collection: Also known as “port-based blood draw,” this option can access blood for sampling through a central line/catheter that is typically in position in patients for other needs. A central line/catheter draw almost always produces an adequate blood sample on a first try if the device is properly managed to avoid contamination of the blood specimen with intravenous fluids, anticoagulants, and so on. The use of central lines/catheters exclusively for blood sampling is the most invasive option and includes some significant risks for patients. Central lines/catheters must be maintained carefully to reduce the risk of thrombosis, sepsis, and infection with MRSA (methicillin-resistant Staphylococcus aureus). The introduction of catheters coated with antimicrobial agents has helped to reduce, but not eliminate, many of these risks.
The technology to facilitate sample collection from a central line/catheter typically involves an access device connected to the sample holder. This makes it possible to collect a sample without the use of a needle. In addition to reducing the risk of exposure of healthcare workers to bloodborne pathogens, this option can also help to reduce the risk of hemolysis which can, in turn, lead to inaccurate measures of potassium levels in blood samples or other erroneous laboratory-test results.
Capillary blood collection: Collection of blood samples from capillaries can be advantageous because capillaries are easily accessible and the process presents only limited risk to the patient. There are important distinctions, however, between capillary and venous blood that can affect sample-analysis outcomes. For example, the levels of certain analytes (including glucose, bilirubin, calcium, and others) in capillary blood and venous blood are measurably different. In addition, the volume of capillary blood is limited, often resulting in a maximum 600-uL draw. While this may be sufficient for hematology testing, it may not be sufficient for large panels used in chemistry testing.
Due to the small size of capillary-blood tubes and the low sample volume, these devices cannot usually be tested on instruments using the automated-testing mode. Instead, these samples must often be processed manually, which results in more steps, increasing the risk of human error as well as the risk of transmission of bloodborne pathogens. Smaller-size tubes also cannot accommodate a label that can capture all needed information (e.g., the patient’s name and unique identifier number, specimen-collector’s name/initials, date and time of specimen collection, instrument barcode). Without all necessary information available on a label, the risk that a sample could be misidentified can be significantly higher.
Efforts to collect and store smaller samples in standard-size tubes, on the other hand, can result in an inappropriate ratio of blood sample to active agents in the tube, potentially compromising the sample or affecting testing results. In addition, automated processing equipment may still not be able to access a smaller volume sample contained in a standard-size tube.
Recent advances in hematology-tube design to support capillary-blood collection are having a widespread impact on patient and clinician experience, reducing the risk of collection and processing errors while increasing the speed to results. Specially designed hematology tubes for capillary collection can hold a smaller sample size in a standard-size tube shell. Pierceable caps make it possible for capillary samples to be processed and tested on most automated instruments. The tube can also accommodate a full-size label.
Patient and clinician impact
The important news for patients and laboratory teams is that recent advances in technology related to blood-sample collection are improving standard of care without requiring either additional manual procedures or a significant investment in staff training or equipment. Using the microtube for automated process is an example. This one advancement in product design and technology can make it more likely for collection to produce an acceptable specimen for all patients, including offering an important alternative for DVA patients. These products can reduce the number of processing and testing steps, with corresponding improvements in turnaround times, and patient and healthcare worker safety.
See related article Challenges of the oncology draw
Ana Stankovic, MD, PhD, MSPH, is worldwide vice president of Medical and Scientific Affairs and Clinical Operations at BD Diagnostics-Preanalytical Systems, the manufacturer of the BD Microtainer MAP Microtube for Automated Process with K2EDTA, a standard-size blood-sample collection tube for use in capillary-blood collection.