COVID-19’s impact on testing practices for sexually transmitted infections
In April 2022, the Centers for Disease Control and Prevention (CDC) released its 2020 STD Surveillance Report, based on data that “provide(s) the clearest picture yet of COVID-19’s impact on the U.S. STD epidemic.” 1
According to the CDC, reported cases of sexually transmitted diseases (STDs) declined during the first few months of the pandemic, which the agency attributes to a drop in testing. Because healthcare facilities were overwhelmed with COVID-19 patients, and others temporarily shut their doors, there were fewer places for individuals to turn for STD screening.
Comparing lab reporting of STDs from April 2019 to April 2020:
- 30% decrease overall in total number of positive STD test results via electronic laboratory reporting (ELR), 40% drop in positive tests via paper reporting
- 38% decrease in positive reactive syphilis serologies via ELR, 49% via paper
- 32% decrease in positive chlamydia results via ELR, 40% via paper
- 15% decrease in positive gonorrhea results via ELR, 34% via paper 2
The CDC data shows a resurgence in STDs by the end of 2020, as testing once again became widely available, with reported cases of gonorrhea, syphilis, and congenital syphilis surpassing 2019 levels.
“The COVID-19 pandemic put enormous pressure on an already strained public health infrastructure,” said Jonathan Mermin, MD, MPH, Director of CDC’s National Center for HIV, Viral Hepatitis, STD, and TB Prevention. “There were moments in 2020 when it felt like the world was standing still, but STDs weren’t. The unrelenting momentum of the STD epidemic continued even as STD prevention services were disrupted.”
Under its Clinical Prevention Guidance, the CDC describes five major strategies for the prevention and control of STDs - also referred to as sexually transmitted infections (STIs) - with three focused on testing and diagnosis.
- Accurate risk assessment and education and counseling of persons at risk regarding ways to avoid STIs through changes in sexual behaviors and use of recommended prevention services
- Pre-exposure vaccination for vaccine preventable STIs
- Identification of persons with an asymptomatic infection and persons with symptoms associated with an STI
- Effective diagnosis, treatment, counseling, and follow-up of persons who are infected with an STI
- Evaluation, treatment, and counseling of sex partners of persons who are infected with an STI11
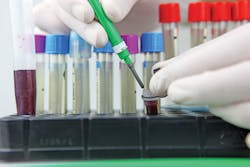
With STD screenings on the rise, clinical labs are faced with higher volumes of tests to process with fewer staff members and shortages of laboratory consumables, including blood specimen collection tubes.
Manufacturers of laboratory equipment and supplies share their insights on the challenges faced by labs in screening for STDs and steps labs can take to diagnose patients with greater accuracy and efficiency.
Process automation
“The pandemic aggravated the preexisting laboratory staffing shortages brought on by overdemand and burnout,” said James Walker, VP of MDx Core & Women’s Health and Cancer, BD. “Plus, the pandemic saw many more experienced laboratorians retiring. And on top of that, the pandemic forced many people to postpone health screenings.”
“Now, as patients get back to doctors’ offices to catch-up on delayed screenings, we’re likely to see testing volumes rise to pre-COVID numbers or higher,” Walker continued. “That means those same already short-staffed labs will be—forgive the word choice—sorely tested themselves. It’s a perfect storm of reduced staff—and less senior staff—coupled with higher demand as well as supply chain challenges to secure inventory of the actual tests themselves.
Walker says labs need to take full advantage of automated- and AI-driven or supported processes. He notes how remote system monitoring, redundancy of sub-systems and long walkaway times can help reduce the likelihood of human error while helping meet the demand challenges presented by staffing shortages and increased patient demand on testing resources.
“Integrated automation of the pre-analytical workflow, as well as onboarding capacity of reagents and specimens, enable delivery of several hundred more test results than a human worker can produce with limited intervention – and in a much shorter timeframe,” Walker added.
Michelle Garsha, President, Diagnostic Solutions at Hologic, says the company is helping labs achieve greater efficiency, decrease turnaround times, and expedite results through continued implementation of its Panther system, which provides adaptable workflow options and a consolidated testing menu that help streamline lab operations. Hologic now has over 3,100 Panthers installed globally.
“As labs grapple with staff shortages, continued demand for COVID-19 testing and more, ensuring laboratory workflows are set up to run tests efficiently and accurately is key. Hologic’s Panther system, a fully automated, integrated molecular testing platform with true sample-to-result automation, adaptable workflow options and a consolidated testing menu, substantially reduces hands-on time for laboratories by allowing for random and continuous access, without batch restrictions and in rapid turnaround time, which can greatly help address the challenges of the lab landscape today.”
Overcoming supply shortages
As the American Society for Clinical Pathology (ASCP) states in a 2022 press release: “Shortages of specimen tubes, personal protective equipment, and other common laboratory consumables threaten access to all aspects of diagnostic testing.”[1]
Garsha comments on continued supply and staffing shortages and the impact on U.S. labs:
“Over the course of the COVID-19 pandemic, an influx of COVID-19 tests meant an increased demand for common laboratory equipment such as swabs and test tubes, among other supplies. Early on, it was clear that collection devices would need to keep up with demand.”
In response to this demand, Hologic gained approval for the Aptima Multitest swab for use with its SARS-CoV-2 assays to help alleviate supply constraint by offering additional swab options for laboratories to choose from based on their inventory.
Hologic also gained approval for Panther Trax, the latest addition to the Panther Scalable Solutions portfolio of products, offering even greater lab automation by physically linking multiple Panther instruments together into a single workcell that allows labs to increase testing volumes without increasing staff.
“As the COVID-19 pandemic begins to wane and we approach an endemic phase of the virus, Hologic continues to monitor lab issues and supply and to ensure lab needs are met at all stages of this pandemic,” Garsha added.
Sample transport
When patients are waiting hours, days, or even weeks for the results of STD tests, the last thing they want to hear is that the testing was inconclusive and will have to be performed again. Preservation of the specimen during transport from the point of testing to the lab for processing is critical to accurate test processing.
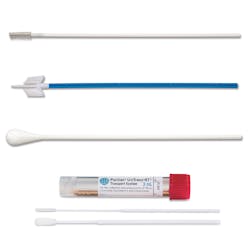
“Efficient collection and accurate results are critical aspects of all patient testing,” said Virginia Templet, Director of Marketing, Puritan Medical Products. “When testing for STIs that can be identified through specimen collection with a swab, consider Puritan’s UniTranz-RT universal transport media product. This medium is available in 1ml and 3ml vials or combined with a flock swab, designed with the patient in mind. For your gynecological patients, choose Puritan’s large rayon tip swab, Histobrush and the Rovers family of cervix brushes, all from Puritan.”
Some STD viruses are more susceptible to damage during transport. One of the most common STDs, the herpes simplex virus (HSV), is highly sensitive to desiccation and pH inactivation, and the virus infectivity is heat labile. Therefore, the “specimen should also be transferred quickly to a diagnostic virology laboratory on ice (+4°C).”4
HPV Testing
As the Centers for Disease Control and Prevention (CDC) reports, Human Papillomavirus (HPV) “is so common that nearly all sexually active men and women get the virus at some point in their lives.”5 In the U.S., there are an estimated 42.5M HPV infections - new or existing – at any given time.6
“It’s important to consider HPV when talking about STI screening because almost all cervical cancer is caused by high-risk HPV,” said Walker. “There are 14 high-risk HPV genotypes, and each high-risk genotype is associated with a different level of risk of progression to cervical pre-cancer and cancer. BD Onclarity HPV Assay is the only FDA-approved assay with extended genotyping, reporting six high-risk HPV genotypes individually, including HPV 31. The assay with extended genotyping, is a more precise, accurate way to measure a woman’s risk for developing cervical pre-cancer and cancer.”
Syphilis testing
While STDs, such as syphilis and gonorrhea, have been widely recognized for centuries, clinical labs still struggle with the accuracy and efficiency of diagnostic tools. With the rise in highly infectious primary and secondary (P&S) syphilis rates since a historic low in 2001,7 researchers are focusing on ways to achieve earlier diagnosis.
A Comparative Analysis of Molecular and Serologic Testing for Primary Syphilis, published in the Frontiers in Cellular and Infection Microbiology in April 2021, describes how “syphilis serology is imperfect and requires interpretation of multiple tests while molecular diagnostics allows for potential yes-no identification of highly infective, primary anogenital lesions.” 8
The researchers performed a retrospective analysis of adult patients with anogenital lesions who were screened for syphilis and herpes simplex (HSV) 1/2 in Alberta, Canada using polymerase chain reaction (PCR) to evaluate Tp-PCR versus serology to diagnose primary syphilis.
The researchers concluded that “molecular testing using Tp-PCR for primary syphilis appears to be a highly specific test with low sensitivity that is, therefore, most useful in confirming the diagnosis rather than as a screening test.” They added, “Concurrent testing with syphilis serology remains necessary to ensure all cases are identified to manage the worsening epidemic and further work is required for the development of superior diagnostic assays that are both sensitive and specific.”
Chlamydia testing
According to the CDC, chlamydia is the most frequently reported bacterial STI in the U.S., with a total of 1,579,885 cases reported in 2020. Chlamydia rates are highest among adolescents and young adults, with almost two-thirds (61%) of all reported chlamydia cases in 2020 among persons aged 15–24 years.[1]
“It’s important to consider that delays in care during 2020 most likely resulted in many underreported cases particularly because STIs like chlamydia are often asymptomatic,” said Garsha. “Since many STIs have gone undiagnosed and untreated, this could lead to harmful health consequences such as infertility. As patients return to routine care and resume screening, there’s a need to ensure labs are able to keep up with demand to diagnose patients accurately and efficiently as we attempt to curb the spread of STIs.”
Testing for multiple STD diagnosis
The CDC recommends certain populations be screened for multiple STDs. For example, all pregnant women should be tested for HIV, syphilis, and hepatitis B surface antigen (HBsAg), at their first prenatal visit, and hepatitis C virus (HCV) during each pregnancy, except in settings where the HCV infection rate is <0.1%.
“It is critical for labs and healthcare systems to offer STI tests that have a quick time to result and user-friendly techniques for processing,” said Walker.” BD offers the BD CTGCTV2 assay for BD MAX System, a test that simultaneously and separately diagnoses the three most common non-viral STIs: Chlamydia trachomatis (CT), Neisseria gonorrhoeae (GC), and Trichomonas vaginalis (TV).”
Walker says TV is often not included in STI testing, but it should be. According to the CDC, there were more than 2 million TV infections in the U.S. in 2018, but only 30% of those individuals infected develop symptoms.10
“The BD assay diagnoses TV using the highly sensitive CDC-recommend NAAT technology,” Walker explained. “For GC diagnosis, the assay has a dual-target design, meaning detection of both GC genes is needed to produce a positive result. This makes a big difference because it provides confidence in your result, confidence that a positive IS a positive, and that you are providing the physician and ultimately the patient with an accurate result.”
Walker says the GC test is run on the BD MAX System, a benchtop instrument that can process 24 samples in about three hours. Plus, the BD CTGCTV2 assay uses a variety of specimen types: clinician and self-collected vaginal swabs (in a clinical setting), urine, liquid-based cytology (CT & GC only), and endocervical swabs.
The Hologic Aptima Multitest Swab can run four tests from one tube and detect up to seven infections and disease states with just one vaginal swab. Garsha says Multitest swab not only provides better collection experience for healthcare providers and patients, but with a penetrable cap and the ability to directly load, it greatly improves laboratory experience by reducing human error and repetitive motion injuries, eliminating manual uncapping, recapping and specimen transfer and more—all of which are beneficial to ensuring labs are accurately and efficiently helping diagnose STIs.
“Another way labs can be sure about the accuracy of their tests is by using the latest testing technology such as molecular Nucleic Acid Amplification Tests (NAATs), which allow for detection with a high degree of sensitivity and specificity and have numerous advantages over conventional methods of testing,” Garsha added.
Looking ahead
Preliminary CDC data on STD rates in 2021 reveal a continued increase in infections, specifically for primary and secondary syphilis among adults. Cases among women are up 34% and among men 9%. In addition, syphilis among newborns is up 6%, with 2,268 cases already reported in the preliminary 2021 data, which the CDC will continue to report through the fall of 2022.11
Laboratories are just beginning to see the front end of increased STD screenings coming out of the pandemic and will likely experience higher volumes in the months and years ahead as more patients resume regular screening.
As the CDC states in its April 12, 2022 press release: “There is much to be done to rebuild, innovate, and expand STD prevention and control in the United States—and this will require many groups working together, including local healthcare systems, clinics, and community-based organizations; public and private sectors; health care providers; and public health workers.”12
References:
- New data suggest STDs continued to increase during first year of the COVID-19 pandemic, CDC, April 12, 2022, https://www.cdc.gov/nchhstp/newsroom/2022/2020-STD-surveillance-report-press-release.html
- How the COVID-19 Pandemic has Impacted Sexually Transmitted Diseases (STD) Programs, CDC, https://www.cdc.gov/std/program/327850-A_FS_COVID19_STD_Impact_508_FINAL.pdf
- New data suggest STDs continued to increase during first year of the COVID-19 pandemic, CDC, April 12, 2022, https://www.cdc.gov/nchhstp/newsroom/2022/2020-STD-surveillance-report-press-release.html
- LeGoff, J., Péré, H. & Bélec, L. Diagnosis of genital herpes simplex virus infection in the clinical laboratory. Virol J 11, 83 (2014). https://doi.org/10.1186/1743-422X-11-83.
- Human Papillomavirus (HPV) Statistics, CDC, https://www.cdc.gov/std/hpv/stats.htm
- Sexually Transmitted Infections Prevalence, Incidence, and Cost Estimates in the United States, CDC, https://www.cdc.gov/std/statistics/prevalence-2020-at-a-glance.htm
- National Overview of STDs, 2020, CDC, https://www.cdc.gov/std/statistics/2020/overview.htm#Syphilis
- Shukalek, Caley & Lee, Bonita & Fathima, Sumana & Chu, Angel & Fonseca, Kevin & Somayaji, Ranjani. (2021). Comparative Analysis of Molecular and Serologic Testing for Primary Syphilis: A Population-Based Cohort Study. Frontiers in Cellular and Infection Microbiology. 11. 579660. 10.3389/fcimb.2021.579660. https://www.researchgate.net/publication/351086070_Comparative_Analysis_of_Molecular_and_Serologic_Testing_for_Primary_Syphilis_A_Population-Based_Cohort_Study
- Screening Recommendations and Considerations Referenced in Treatment Guidelines and Original Sources, CDC, https://www.cdc.gov/std/treatment-guidelines/screening-recommendations.htm
- Trichomoniasis – CDC Fact Sheet, CDC, https://www.cdc.gov/std/trichomonas/STDFact-Trichomoniasis.htm
- Preliminary 2021 Data: Syphilis, CDC, https://www.cdc.gov/std/statistics/2020/preliminary2021.htm
- New data suggest STDs continued to increase during first year of the COVID-19 pandemic, CDC, https://www.cdc.gov/media/releases/2022/p0412-STD-Increase.html
Kara Nadeau has 20+ years of experience as a healthcare/medical/technology writer, having served medical device and pharmaceutical manufacturers, healthcare facilities, software and service providers, non-profit organizations and industry associations.
About the Author

Kara Nadeau
has 20+ years of experience as a healthcare/medical/technology writer, having served medical device and pharmaceutical manufacturers, healthcare facilities, software and service providers, non-profit organizations and industry associations.