Companion diagnostics: an emerging component in personalized medicine
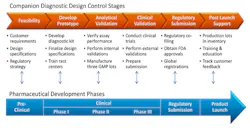
Companion diagnostics is a relatively new area of diagnostics that has significant potential for patients, diagnostic laboratories, diagnostic companies, and pharmaceutical companies. As is often the case with new terminology in any field of knowledge, however, the definition of companion diagnostics is in some flux. The term is used in different ways. I would define companion diagnostics as a process that aligns the regulatory submission of a pharmaceutical with the regulatory submission of a diagnostic to provide information about the efficacy or potential efficacy of the drug in patients. A general scheme of the relationship between pharmaceutical drug development and companion diagnostics design is provided in Figure 1.
Credit: Grace Knutson
More generally, companion diagnostics falls under the broader category of personalized medicine, which is a term that is used frequently today to describe efforts by the medical community to provide patient-tailored solutions for human disease. The potential of companion diagnostics to provide information about an individual patient’s response to a particular therapy allows clinicians and ultimately patients to make decisions on their care based on data about efficacy in addition to the possibility of side effects.
As a laboratorian and pathologist, I am most excited about the fact that companion diagnostics focuses on the mechanism of disease and the potential interventions provided by pharmaceuticals. The vast expansion of molecular, proteomic, and metabolomics data on disease states has allowed the pharmaceutical industry to focus on particular disease targets while the diagnostic community can focus on biomarkers of this activity. This description is distinct from the detection of genes that confer increased risk of disease; the best example of that has been the much-publicized use of BRCA-1,2 testing and the relationship with breast and ovarian cancer. I will comment more on this approach below.
The most significant advantage of the companion process is the ability for diagnostics companies and pharmaceutical partners to form close collaborations to achieve the best outcomes for patients. The pharmaceutical companies benefit by being able to stratify patients into groups that will respond to the particular treatment, hopefully with a minimum of adverse effects. The diagnostics companies benefit by having a defined clinical trial plan that meshes with the design control stages of the device verification and validation. Assuming that the drug moves forward through the regulatory process, which can be a risk assumed by both the pharma and the diagnostics company, the diagnostic is well served by the creation of a defined market that may not have existed prior to the development of the drug. In addition, the pharmaceutical company can benefit from the potentially longer patent life a novel companion diagnostic will have if the regulatory agencies require the diagnostic result prior to the initiation of therapy.
“What makes a good companion diagnostic?” That is the overriding question facing the diagnostics industry today. In some cases, such as the CYP2C9 p450 enzyme, genetic polymorphisms define responses to drugs such as warfarin. Detection of these polymorphisms is relatively straightforward and can be determined by a number of different technologies. The presence of the BCR-ABL translocation in CML is another example of a straightforward molecular assay to determine responsiveness to drug therapy (Gleevec).
As drug discovery has become more sophisticated and as disease pathways have become elucidated, however, simple molecular tests may not suffice to provide the necessary information to guide therapy and therapeutic decisions. Diagnostics may need to detect proteins, mRNAs, and cell cycle in combination or multiplexed. A good example is the common use of HER2/neu detection in breast cancer to determine the responsiveness to Herceptin. First, HER2/neu is expressed at low levels on normal breast cancer cells, so quantification of HER2/neu gene or protein “over-expression” is necessary. Second, there is debate as to whether the HER2/neu protein or mRNA is more specific for determining response to therapy.
Commonly, HER2/neu protein staining is performed on breast biopsies (or cores) by immunohistochemistry. Semi-quantification is performed on the tissue followed by a reflex to HER2/neu in situ hybridization for mRNA if the result is equivocal. From a workflow and cost standpoint this requires two separate tests performed from tissue blocks and requires microscopic review by a pathologist. This process can take days before a final result is produced. Newer technologies exist, however, that can directly quantify HER2/neu protein and mRNA simultaneously in a matter of hours at the same or lower cost (Figure 2).
Credit: A. Chagrin, K. Shults, B. Patterson
In summary, this is an exciting time in diagnostics, in part because of the challenges and opportunities of companion diagnostics. The highly publicized story of actress Angelina Jolie, who chose to undergo a preventive double mastectomy after genetic testing for the BRCA mutation, has put before the public both the advantages and current limitations of the new diagnostics; Jolie and other women with a similar genomic profile face difficult personal decisions because we as a diagnostic community have been unable to provide enough information about disease and disease progression to support less invasive alternatives. This is a call to arms to the diagnostic industry to get creative, innovate, and come up with more complete solutions when someone has a risk of disease. Highly invasive procedures should be the last resort. We should also be creative in developing cost-effective companion diagnostics so that a higher proportion of patients can afford to be given the information they need to manage their health.