Blood glucose monitoring looks at patterns in the fluctuation of blood glucose (sugar) levels that occur in response to diet, exercise, medications, and or pathological processes associated with blood glucose fluctuations such as diabetes. Unusually high or low blood glucose levels can potentially lead to acute and/or chronic, life-threatening conditions. Blood glucose level (BGL) or blood sugar level (BSL) monitoring undertaken in the home/community are often referred to as capillary blood glucose (CBG) tests, while blood glucose tests carried out at clinical facilities may include CBG and (plasma glucose) venous blood tests.1 The American Diabetes Association (ADA) generally recommends the following target blood sugar levels: between 80 and 130 milligrams per deciliter (mg/dL) or 4.4 to 7.2 millimoles per liter (mmol/L) before meals; less than 180 mg/dL (10.0 mmol/L) two hours after meals.2
Pathophysiology
Most food products contain complex carbohydrates that are broken down to supply energy to the cells in our body. Once ingested, carbohydrates are broken down in the gastrointestinal system into simpler sugars such as glucose. In the small intestine, glucose molecules are absorbed into the bloodstream and transported to cells across the body and to the liver. Insulin is produced by the beta cells in the pancreas in response to elevated blood glucose levels.1
In conditions like diabetes, there is either a lack of insulin or the body does not appropriately respond (otherwise called insulin resistance) to the actions of insulin (to facilitate cellular uptake of glucose or storage of excess glucose). Patients with impaired blood glucose levels and impaired fasting blood glucose are at high risk for developing diabetes. Patients are diagnosed with diabetes if their BGL’s are high. Some organs such as the brain, kidneys, liver, and red blood cells do not have insulin receptors and do not require insulin for the uptake of glucose. These organs, especially the brain, are significantly affected by acute, chronic, and/or recurrent drops in blood glucose levels and are associated with significant morbidity.1
Insulin is used in the management of type 1 diabetes and some cases of type 2 diabetes. Insulin therapy has a well-known adverse side effect of hypoglycemia if its administration is not managed effectively. Patients with insulin-dependent diabetes benefit from regular blood glucose monitoring.1
Diagnostic tests
Capillary blood glucose test
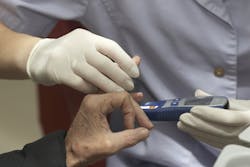
A capillary blood glucose test is a blood drop sample usually collected from a fingertip prick. Blood samples can also be sourced from alternate sites such as the earlobe, heel, forearm, palm. Alternate site testing provides similar results to finger-prick testing, especially when fasting and within two-hours post-meal. Check with the manufacturer of the glucometer if the machine can be used for alternate site testing.
Equipment used includes a lancet used to prick the skin, glucometer, and test strips. Glucometers require a very small sample of blood (from 0.3 to 1 microliter) and have a range of features, including Bluetooth capabilities that synchronize data with paired applications (apps) on smartphones. These machines and apps record data and provide trends in glucose measurements undertaken. Further, some apps also provide options to record diet, medications used, and types of physical activity undertaken, which may be useful to the healthcare practitioner when managing the care plan for the patient with diabetes.
One disadvantage of a CBG test is the accuracy of the results is dependent on the clinical presentation of the patient, i.e., it may not be very reliable in patients with hypoglycemia, anemia, altered hematocrit, hypotension, or those who are critically ill. Older machines may need calibration with test strips, and results could be compromised if the calibration is not undertaken appropriately.
Venous blood sample
The venous (plasma) blood sample is collected via venipuncture by a phlebotomist, medical laboratory scientist, nurse, etc. The equipment used for venipuncture includes collection tubes, needles, tourniquet, wipes/swabs, gauze, bandages, gloves, laboratory forms and blood specimen labels, transportation bags, and sharps container. The most accurate blood glucose measurements are obtained from venous specimens that are analyzed in a clinical laboratory.
Venous blood samples are considered accurate measurements of blood glucose and are superior to the capillary blood glucose test. There are some slight risks associated with venipuncture that may include pain, excessive bleeding, light-headedness, fainting, nerve damage, hematoma (accumulation of blood under the skin), and infection.
Continuous glucose monitoring
Continuous glucose monitoring (CGM) involves insertion or application of a water-resistant disposable sensor on the abdomen or back of the upper arm. The sensor can be scanned with a reader, which displays the patient's current glucose level. Seeing glucose levels in real time can help individuals make more informed decisions throughout the day about how to balance food, physical activity, and medicines. Individuals can also review glucose changes over a few hours or days to see trends. Data from the CGM device can be shared with family and care providers via a smartphone application, and the apps are often capable of sending alerts, such as for hypoglycemia, a particular benefit during the night while sleeping. Some CGM's can work with compatible insulin delivery devices and can stop insulin delivery if the machine predicts and or recognizes a drop in blood sugar level. However, glucose is first seen in the blood before it is seen in interstitial fluid, which the CGM measures. As such, the CGM may not always be a reliable indicator in rapidly changing blood glucose levels.
Hyperglycemia
Etiology of hyperglycemia includes:
- Inadequate insulin administration in patients with type 1 diabetes
- Insulin resistance with type 2 diabetes, which inhibits glucose metabolism
- Stress-related experiences (such as critical illness) inducing glycogenolysis and gluconeogenesis
- The dawn phenomena where there is a surge in blood glucose levels
Symptoms of hyperglycemia include polyuria (increased and frequent urination), polydipsia (increased thirst), blurred vision, headache, fatigue, and glucosuria. Acute symptoms of hyperglycemia are not usually seen at levels below 14 mmol/L or 250 mg/dl.1
Episodes of hyperglycemia for an extended period could lead to either diabetic ketoacidosis or hyperglycemic hyperosmolar state. Diabetic ketoacidosis is a life-threatening scenario where an individual could potentially go into a state of coma from a lack of insulin production. Individuals may also have symptoms of fruity odor (from the ketones being produced in the body as a result of fat metabolism), dry mouth, shortness of breath, nausea, or vomiting.1,3
In the hyperosmolar state, a rare condition seen in patients with type 2 diabetes, the body in its attempt to get rid of the high glucose levels in the blood, produces large amounts of urine causing life-threatening dehydration and potentially coma.1,3
Long-term high blood glucose levels could potentially delay wound healing, damage nerves (peripheral neuropathy), and damage organs such as the eyes (diabetic retinopathy), kidneys (renal failure), brain (stroke), and heart (myocardial infarction).1
Hypoglycemia
Hypoglycemia is a condition in which a person’s blood sugar (glucose) level is lower than the standard range. Symptoms of hypoglycemia are seen when low blood glucose levels deprive the body of essential fuel to sustain life. The most common reason for low blood sugar is a side effect of medications used to treat diabetes.1,4
Symptoms of hypoglycemia include sweating, irregular heartbeat, blurred vision, lightheadedness, or difficulty concentrating. If individuals do not recognize the onset of symptoms of hypoglycemia, they may put themselves at risk for injury. As hypoglycemia worsens, symptoms include loss of coordination, confusion, and blurred vision.1,4
Emergent treatment to restore normal blood glucose levels is imperative as certain organs (e.g., brain) do not store glucose and need a constant supply of blood glucose to sustain life. Antidiabetic therapy needs reevaluation when BSL falls below 5.6 mmol/liter (100 mg/dl), and modification of antidiabetic therapy is essential if BSL drops below 3.9 mmol/liter (70 mg/dl).1
Conclusion
Blood glucose monitoring is an essential part of management of patients with diabetes. Having very high or very low levels of blood glucose could impair cellular function and may be lethal if not managed appropriately. Patients need education on the importance of regulating diet, exercise, and medications to prevent acute and or chronic complications that are seen in extreme blood glucose fluctuations in conditions like diabetes. The use of glucose management protocols, with nurse-initiated treatment protocols, is ideal for the management of hyperglycemia and hypoglycemia in the hospital setting.1
REFERENCES
1. Mathew TK, Tadi P. Blood Glucose Monitoring. In: StatPearls. Treasure Island (FL): StatPearls Publishing; August 8, 2022.
2. American Diabetes Association Professional Practice Committee. 6. Glycemic targets: Standards of medical care in diabetes-2022. Diabetes Care. 2022;45(Suppl 1):S83-S96. doi:10.2337/dc22-S006.
3. Hyperglycemia in diabetes. Mayo Clinic. Published August 20, 2022. Accessed March 1, 2023. https://www.mayoclinic.org/diseases-conditions/hyperglycemia/symptoms-causes/syc-20373631.
4. Hypoglycemia. Mayo Clinic. Published May 4, 2022. Accessed March 1, 2023. https://www.mayoclinic.org/diseases-conditions/hypoglycemia/symptoms-causes/syc-20373685.