Influenza during the time of COVID-19
For a printable version of the February CE Story and test go HERE or to take test online go HERE. For more information, visit the Continuing Education tab.
LEARNING OBJECTIVES
Upon completion of this article, the reader will be able to:
- Compare and contrast the characteristics of influenza A and influenza B in past pre-COVID-19 flu seasons.
- Discuss the impact of COVID-19 and mitigation measures on the severity of the 2020-2021 influenza season.
- Discuss the societal and individual actions that might impact the severity of the 2021-2022 flu season.
- Describe the role of rapid diagnostic testing in managing both COVID-19 and flu outbreaks.
In advance of the 2020-2021 influenza in the U.S., public health officials in the Southern Hemisphere provided reports regarding their first influenza season since the official onset of the COVID-19 pandemic. These records indicated a profound drop in the incidence of influenza and other respiratory viral infections compared to previous seasons. This was believed due, in part, to the implementation of nationwide mitigation programs, including social distancing, mask wearing, restrictions on mass gatherings, travel restrictions, and other behavioral precautions that were aimed at limiting the spread of SARS-CoV-2.
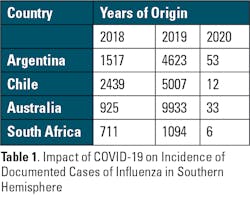
By the end of the Southern Hemisphere’s 2020 winter season, there was a dramatic decline (>99%) in incidence of PCR-confirmed cases of influenza in Australia, South Africa, and across South America (Table 1).1 Similarly, the traditional influenza season never developed again in the ensuing 2021 winter season with case levels at 10% or less than typically encountered in most regions of the Southern Hemisphere.2
Influenza in the USA from 2015 to December 2021
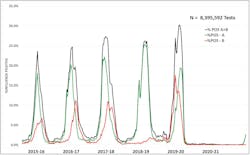
Forecasting the impact of an approaching flu season is a profoundly difficult task. Data generated in the Southern Hemisphere were certainly clues to what might occur in the U.S. In addition, using the data available from the Centers for Disease Control and Prevention (CDC),3 epidemiologists were able to examine historical influenza seasonal outcomes and trends that could provide clues about the forthcoming influenza season. The influenza data spanning the period from the onset of the 2015-2016 season (week 40) to December 2021 (week 48) is presented in Figure 1.
The CDC data presented here is comprised of influenza test results provided by over 400 clinical laboratories that comprise the nationwide WHO/NREVSS laboratory network.4 The positivity rates for influenza types A+B combined, or individually, are depicted by respective colors, as shown, and range from about 1% (types A+B combined) to as high as 30%. This figure contains an immense amount of data, so let’s look at some of it more closely.
USA 2016 and 2017 influenza epidemic seasons
The 2016-17 and 2017-18 seasons in Figure 1 were “typical” and show, first, the seasonal arrival of influenza A (green), soon followed by influenza B (red). Conventionally, influenza B reaches its seasonal peak about 5 to 7 weeks after influenza A. This profile is consistent with preceding influenza seasons going back several years.
USA 2018, 2019, and 2020 influenza epidemic seasons
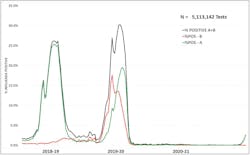
Did this pattern persist into the subsequent three seasons? The answer is “No.” The subsequent three seasons each had unusual and distinct profiles, as shown in Figure 2. The 2018-19 epidemic in the U.S. was characterized by a particularly strong influenza A season (green) accompanied by remarkably low levels of influenza B (red) with positivity rates always well below 3% across the nation and never peaking anytime during that year’s entire epidemic.
Then came the 2019-20 season, with influenza B arriving before influenza A for the first and only time in any season, going back, at least, to 2008 and achieving a nearly 2-fold higher percent positivity peak than any observed in the preceding three seasons.
As the COVID-19 pandemic arrived, reports demonstrated an abrupt end to the 2019-20 influenza season in the United States, as shown graphically by the sharp, rapid fall of the influenza positivity rates for influenza types A and B in February-March 2020. Indeed, in the subsequent winter, 2020-21, we can argue that there was no influenza season in North America with influenza positivity rates for types A+B combined rarely exceeding 2% for nearly 20 months.
As shown in Figure 3 below, despite the low influenza positivity rates lasting for 19 months, the number of influenza tests climbed slowly, but steadily, through the largely vacant 2020-21 influenza season. Although episodic cases of influenza were reported across the nation, much of this testing was likely stimulated by the similarity of symptoms for influenza-like-illness (ILI) and COVID-like-illness (CLI). This profile continued until the end of October 2021 when the influenza A positivity rate itself began to rise (see green line in Figures 1 and 2).
Dramatic decline in influenza-related hospitalizations and deaths in U.S.A
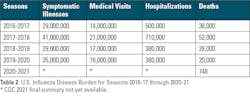
The dramatic decline in positive influenza cases, first reported in the Southern Hemisphere, and observed in the United States, thereafter, profoundly impacted hospitalization and influenza-associated death rates across the nation (Table 2).5 Although the CDC’s full report for the 2020-2021 season is not yet available, participating laboratories have reported testing respiratory specimens from approximately 1.3 million patients of which only 2,136 (0.02%) were positive; there were 748 deaths — only 2% of the average number of deaths for the previous four seasons, according to preliminary reports.10 What factors influenced these profound changes in influenza seasons across the globe?
Factors influencing the decline of influenza in the 2020-2021 season
- Behavioral and societal factors. Most epidemiologists agree that the continued behavioral and societal precautions (Table 3) against the spread of COVID-19 have very likely reduced the appearance and spread of influenza, as well as other respiratory pathogens in the U.S.6
- Case isolation, contact tracing, quarantine. In addition, actions by state public health officials to promote and assist in COVID-19 case isolation, such as contact tracing and quarantining of those exposed, have also likely contributed to the decline in influenza.7
- Pre-existing herd immunity and vaccinations. Before the pandemic, there already was an existing influenza immunity, due to previous influenza infections and influenza immunizations8 in the U.S. The combination of this pre-existing herd immunity against influenza and the behavior and societal factors employed to reduce COVID-19, may have reduced influenza cases even further.9,10
- Reduced test rate for influenza. Some researchers have argued that the reduced influenza burden is a false perception created by declining influenza tests rates. However, ongoing work by the World Health Organization (WHO) demonstrates that testing rates at sentinel sites remain high, providing for an accurate assessment of influenza burden worldwide.11
- Delta and Omicron variants. The arrival of the Delta variant (December 2020) in the U.S., and the growing number of breakthroughs in vaccinated populations, stimulated Americans and their government to reassert mitigation efforts to prevent spread of respiratory disease. Most recently, the arrival of the highly transmissible Omicron variant (November 2021) will likely stimulate similar or even more aggressive steps. The re-implementation of these precautions could impede the arrival of an influenza epidemic again this winter.12,13
Factors favoring a possible return of influenza this winter in the U.S.A.
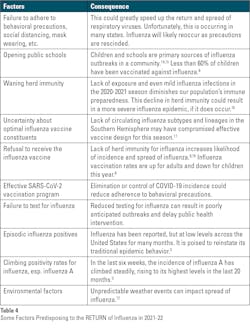
Obviously, trying to predict what will transpire with influenza this year is a formidable challenge. Even before the arrival of COVID-19, we experienced two very unusual and unpredictable influenza seasons that deviated significantly from previous seasons. As such, there is a growing list of factors that suggest a potential return of influenza this coming season (Table 4).
The fact that influenza and SARS-CoV-2 share so many common signs and symptoms makes differential diagnosis a critical element to effective disease management. Treatments for each pathogen are available, including monoclonal antibody therapy, and recent and other forthcoming emergency use authorizations from the U.S. Food and Drug Administration (FDA) of new oral drugs. However, the timing of therapeutic intervention is very important. Often, the windows for effective therapy are short and require administration, as early as possible, following onset of symptoms. In addition, we know that, should influenza and COVID-19 both circulate at high levels in the same community, co-infections of influenza and SARS-CoV-2 can occur — with strong negative impact on patient morbidity, mortality, and indisputable need for intense medical interventions.
The availability of high-quality rapid point-of-care diagnostic tests is critically important as the traditional respiratory virus season continues. Perhaps even more important, the competent application of telemedicine, digital health, and at-home COVID-19 tests could have a profound impact on potential resurgence of influenza infections, in the midst of the ongoing COVID-19 pandemic. Distinguishing an ILI patient from a CLI patient is a challenge, but this must be done competently and quickly to save lives. A negative at-home SARS-CoV-2 test for a symptomatic patient must be followed up with an influenza test if a valid influenza season develops. A rapid multiplex test that detects all three viruses would be an excellent alternative — especially if SARS-CoV-2 and one or more influenza types were prominent in a region.
What can we expect this coming Influenza season?
- COVID-19 or influenza or both illnesses will be present.
- The incidence of either, or both, will likely vary dramatically between different regions in the U.S., based on personal and societal behaviors and on environmental factors in different states.
- With onset of ILI and CLI symptoms, there will be uncertainty about the diagnosis without testing for both influenza and COVID-19.
- Physicians will want to test for both viruses — either one at a time or both simultaneously. The test results could enable prompt therapeutic intervention for either disease.
- If testing separately, a positive test for one cannot rule out a co-infection by the other. Although rare, the consequences of missing a dual infection can be devastating.
- For over-the-counter test options, the ability to test for both viruses in the home setting will be an advantage for the patients and members of the household.
- Children will need to be tested if symptomatic or asymptomatic. It is likely that many will be infected in schools. They may have little or no symptoms, but some will shed virus. Serial at-home testing will likely become much more common.
- Depending on environmental conditions, influenza could strike early this winter, especially in areas with high humidity and warmth.
Closing
Making any forecast, as shown with the above background, is almost impossible. But in the U.S., we are poised with a number of excellent platforms for COVID-19 and influenza diagnosis. Over 267 NAATs and 41 rapid antigen tests have received EUAs for COVID-19. The serial use of rapid antigen tests, particularly multiplex tests for detection of influenza viruses and SARS-CoV-2, in POC settings and/or at-home, will continue to give physicians and public health an early warning, enabling early treatment for influenza and for COVID-19 patients, while keeping our public health agencies informed of outbreaks.
REFERENCES
- Servick K. Coronavirus creates a flu season guessing game. Science. 2020;369(6506):890-891.
- Kausha N. Southern Hemisphere Seasonal Influenza. Outbreak Observatory. https://www.outbreakobservatory.org/outbreakthursday-1/9/16/2021/southern-hemisphere-seasonal-influenza. Published September 16, 2021. Accessed January 3, 2022.
- United States WHO Collaborating Laboratories and NREVSS Influenza Testing Data https://www.cdc.gov/flu/weekly/fluviewinteractive.htm. Accessed January 3, 2022.
- CDC. Dec. 2021. The National Respiratory and Enteric Virus Surveillance System (NREVSS). https://www.cdc.gov/surveillance/nrevss/labs/list.html. Updated October 14, 2021. Accessed January 3, 2022.
- CDC. Disease Burden of Flu. Dec.2021. https://www.cdc.gov/flu/about/burden/index.html. Accessed January 3, 2022.
- Feng L, Shang T, Wang Q, Xie Y, Peng Z, Zheng J. et al. Impact of COVID-19 outbreaks and interventions on influenza in China and the United States. Nat Commun. 2021 May 31;12(1):3249. doi: 10.1038/s41467-021-23440-1.
- Fetzer T Graeber T. Measuring the scientific effectiveness of contact tracing: Evidence from a nature experiment. Proc Natl Acad Sci U S A. 2021 Aug 17;118(33):e2100814118. doi: 10.1073/pnas.2100814118.
- CDC. 2021-2022 Flu Season Summary. https://www.cdc.gov/flu/season/faq-flu-season-2020-2021.htm#anchor_1627000324276. Updated October 25, 2021. Accessed January 3, 2022.
- Lee K, Hawre J, Raviotta J, Krauland M, Zimmerman R, Burke D, Roberts, M. Predicting the impact of low influenza activity in 2020 on population immunity and future influenza season in the United States. medRxiv. https://www.medrxiv.org/content/10.1101/2021.08.29.21262803v1.
- Krauland M, Galloway D, Raviotta J, Zimmerman R, Roberts M. Agent-based Investigation of the impact of low rates of influenza on next season influenza infections. medRxiv. https://www.medrxiv.org/content/10.1101/2021.08.18.21262185v2. Posted August 26, 2021. Accessed January 3, 2022.
- Rubin R. Influenza’s unprecedented low profile during COVID-19 pandemic leaves experts wondering what this flu season has in store. JAMA. 2021 Sep 14;326(10):899-900. doi: 10.1001/jama.2021.14131.
- Hacisuyleyman E, et alia. Vaccine breakthrough infections with SARS-CoV-2 variants. N Engl J Med. 2021 Jun 10;384(23):2212-2218. doi: 10.1056/NEJMoa2105000.
- Fischer M., et alia. COVID-19 vaccine breakthrough infections reported to CDC-United States, January 1 to April 2021. Morbidity and Mortality Report. May 28, 2021 (70/21)792-793.
- Chao D, Halloran M, Longini I Jr. School opening dates predict pandemic influenza a(H1N1) outbreaks in the United States. J Infect Dis. 2010 Sep 15;202(6):877-80. doi: 10.1086/655810.J.
- Mimura S, Kamigaki T, Takahashi Y, Umenai T, Kudoou M, Oshitani H. Role of preschool and primary school children in epidemics of influenza A in a local community in Japan during two consecutive seasons with A(H3N2) as a predominant subtype. PloS One. 2015;10(5): e012564. doi: 10.1371/journal.pone.0125642.
- Carrillo-Santisteve P, Ciancko B, Nicoll A, Lopalco P. The importance of influenza prevention for public health. Hum Vaccin Immunother. 2012.8(1)89-95. doi.org/10.4161/hv.8.1.19066.
- Tamerius J, Nelson M, Zhou S, Viboud C, Miller M, Alonso W. Global Influenza seasonality: reconciling patterns across temperate and tropical Regions. 2011. Environ Health Perspect. 2011 Apr;119(4):439-45. doi: 10.1289/ehp.1002383.
About the Author

Sushruth K. Reddy, BS
is Associate Director of Scientific Affairs at Quidel Corporation.