Automated slide preparation and interpretation can enhance lab efficiency
With technological advancements in automated hematology analyzers, why do we continue to look at blood smears through a microscope? A thorough review of the blood smear in conjunction with the patient’s clinical picture and automated hematology analyzer results becomes invaluable in the diagnosis and clinical care pathway determination of many disease states, including leukemias and anemias. In order to perform a thorough blood smear analysis, we must start with an impeccably made blood smear.
Reviewing a consistently uniform blood smear throughout a patient’s course of treatment is essential to clinicians as they assess treatment efficacy. Improving consistency in review of manually made blood smears may lead to improved messaging to the clinician, potentially impacting patient care.
There are many challenges to mastering the art of the manual smear and that sought-after feathered edge. One must consider many factors in the process. A quicker push at a higher angle results in a thicker smear. A larger drop of blood results in a longer smear, jeopardizing the quality and location of the feathered edge. The hematocrit of the sample (viscosity) can impact the thickness of the smear, resulting in variation of cell distribution whether a smear is too thick or thin. While the goal is to have the smear cover approximately two-thirds of the slide with a feathered edge at the end, the slightest adjustment of the hands vs. the size of the drop of blood and viscosity of the sample may lead to inconsistencies on the part of even the most practiced laboratorians.
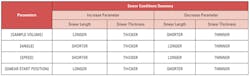
Teaching the manual method requires starting with the basics. This practice can be very laborious and often requires multiple attempts to adjust the blood drop size, angle, and speed of the push. Inconsistencies from length to width and thickness still remain (Table 1).
The benefits of automation
With today’s ever-changing healthcare environment, laboratory managers and directors are challenged to find ways to optimize the utilization of laboratorians and support staff while maintaining and improving turnaround times, and continuing to provide the highest quality patient care. Continuing to perform manual tasks such as preparing manual blood smears takes laboratory professionals away from tasks that require critical thinking that they were trained to do and are relied upon to perform.
Today, there are automated and semi-automated slide makers and slide maker/stainers on the market that can ease the burden on the laboratorian while providing consistency in the smear preparation process.
Semi-automated smear preparation units are designed to provide an improved method of preparing peripheral blood films using the push or wedge technique. They can relieve laboratorians of some of the labor burden, but not all. These units tend to be user-friendly and require very little maintenance. What they are unable to do is self-adjust based on the sample viscosity, creating the possibility that the smear length and thickness may still be inconsistent.
Automated slide makers/stainers with closed tube sample processing provide hands-free, walk-away smear preparation and staining. Automated units drive the consistency needed to ensure uniformly made smears meeting quality, safety and turnaround time requirements. In addition, with direct-to-the-slide printing and barcode reading capabilities, automated smear preparation units are able to imprint the patient’s sample ID and other interfaced demographics directly on the frosted end of the glass slide. This ensures positive patient identification and reduces the chance of transcription and tube mismatch errors that may occur with the manual methods.
Once the slide is identified, the sample is mixed and aspirated. The mixing is consistent from sample to sample, resulting in a uniform cell suspension each time. A drop of blood is then added to the glass slide. Wedge prep/push smear technology is incorporated into the automated smear preparation units so that the smear covers approximately two-thirds of the glass slide, ending in that desired feathered edge.
A step further
Some automated slide makers/stainers take the wedge prep smearing process a step further. With patented technology, some units can incorporate the hematocrit results from the integrated hematology analyzer(s) and apply fine-tune adjustments to each smear. With the hematocrit results driving the behavior of the slide maker, the unit adjusts the speed and the angle at which to push. Each smear produced is of uniform length, width and thickness.
Customizable stain times, another feature of automated slide maker/stainers, allow for the laboratory to achieve the desired coloration not only for whole blood smears but also for body fluid or bone marrow smears. The samples may be loaded while the laboratorian performs other assays. Upon return, completed labeled stained smears are ready for review, thus increasing laboratory efficiencies.
Digital imaging and more
Incorporating digital imaging is the last step to fully automating the slide making and staining process and features cell location and pre-classification. Cell image analyzers provide automation of manual white blood cell differential counts through automatic cell location. Merging results from multiple slides allows differential reporting on the lowest of white blood cell counts, virtually eliminating the need to perform buffy coat analysis. Red blood cell pre-characterization based on the laboratory’s established review criteria and platelet estimate capabilities all drive tech-to-tech consistency while aiding in consistent reporting among staff on even challenging morphologic cases.
Body fluid software found on cell image analyzers is the last piece of the puzzle in automating the smear, stain, and review process in your laboratory. Analyzing cyto-spin smears, the cell image analyzer can automatically perform pre-classification of nucleated cells and captures a digital image of the entire sample area. The laboratorian may also tag areas of interest for follow-up by the pathologist or for collaboration, education, and training.
Remote review stations provide not only a more ergonomic workspace but flexibility for lab staff and for pathologists. Abnormal cells can be reviewed from any networked computer licensed with remote review software, allowing more frequent interaction between the laboratorian and pathologist. This increased collaboration opportunity may lead to faster interpretation and quicker result reporting, enabling the clinician to move forward with diagnosis and treatment.
The industry has come a long way in automating one of the most time-consuming tasks in the laboratory. It is no longer necessary for highly skilled and trained laboratory professionals to stand over the slide prep bench. Staff can now spend more time on the difficult cases that require careful analysis and assessment. Together, automated slide making and staining integrated with automated cell image analysis can enhance the level of service a laboratory provides its clinicians and patients.
Ann Ludwig serves as Group Marketing Manager for Sysmex America, Inc.
About the Author

Ann Ludwig, MT (ASCP)
is Assistant Director, Automation Solutions Marketing at Sysmex America, Inc. Ann is responsible for reference lab strategy and total laboratory automation for optimizing the efficiency, operations, and financial performance of clinical laboratories. With 25 years of clinical marketing and product management experience and lab experience, Ann has successfully launched new and innovative products to the market including Sysmex’s 5th generation slidemaker stainer, the SP-50, and first-of its-kind automated urinalysis platform, the UN-Series, across North America. Ann holds a Bachelor of Science in microbiology from the University of Kansas and a bachelor of science in Medical Technology from the University of Kansas School of Medicine – Allied Health.